In the autumn of 1918, a global influenza outbreak began that would claim more lives than World War I (or the Great War). The war itself, which ended in November 1918, had a significant impact on how the virus spread around the world – and even influenced the name Spanish Flu.
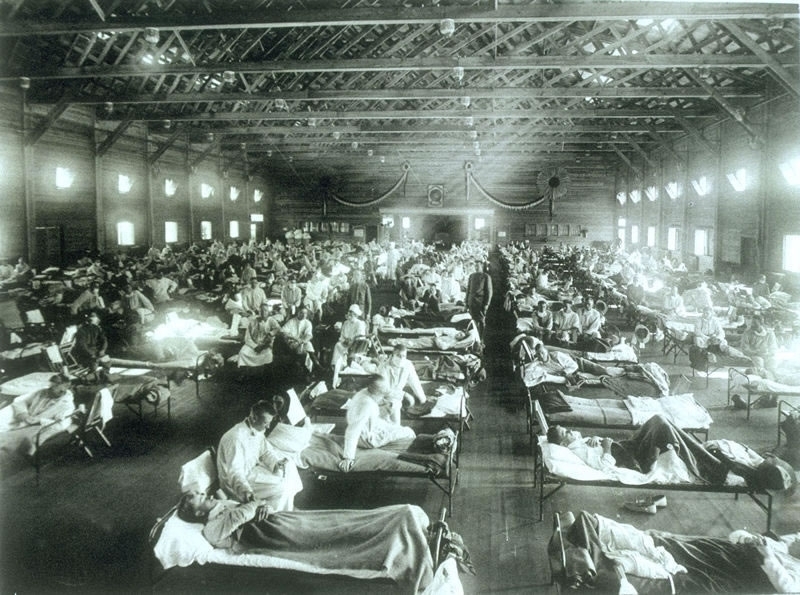
There was nothing particular ‘Spanish’ about the flu: it didn’t begin in Spain and, while the country was badly affected, it wasn’t hit any harder than others. (The first wave spread in US military camps in 1917.)
However, Spain remained neutral during the conflict and its papers freely reported the outbreak. Media in France, the United Kingdom, Germany, the United States and elsewhere played down the impact on their own country in a bid to keep up morale. Newspapers were either directly controlled by national governments or keen to self-censor in the interest of patriotism at a time of war. They all happily reported on events in Spain – leading many to incorrectly presume that the Iberian Peninsula was the epicentre.
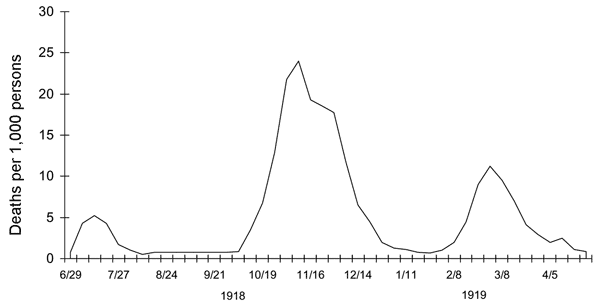
In summer of 1918, the virus spread among military units who lived in cramped quarters. And, as the war ended, surviving solders returned home – bringing influenza with them.
After four gruelling years of conflict, the immediate post-war period was a time for celebration. Public gatherings present an ideal opportunity for infectious diseases to find new victims. This most likely prolonged the second wave of the outbreak.
A third wave in the early spring of 1919 took war-weary populations by surprise, claiming millions more lives. Just as with seasonal influenza, the worst-hit populations were the very old and the very young. However, in comparison to a typical flu epidemic, there was a major spike in the 25-34 age group. Many soldiers who survived the trenches, did not survive the flu. Some returning soldiers shared the lethal virus with their spouses, also helping to push up the fatality rate in young adults.
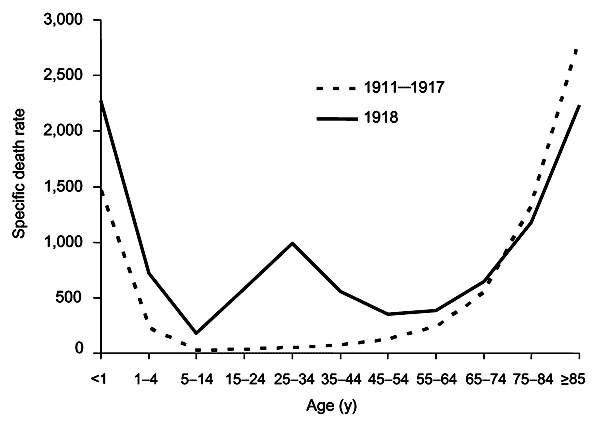
There are a number of other reasons why the proportion of deaths among young adults was higher than normal. For one thing, the older population had partial immunity from the 1889-1890 flu pandemic (known as Russian flu).
The virus has also been shown to have triggered what is known as a ‘cytokine storm’ – an immune response that can be particularly severe in those with stronger immune systems.
The worst-affected group of all were pregnant women. Of the pregnant women who survived, over one quarter is estimated to have lost the child.
(Pregnant women are the #1 priority for flu vaccination, according to the WHO.)
During the 1918-1919 pandemic, researchers tried to develop a vaccine. According to the History of Vaccines project, a number of vaccines were tested against Bacillus influenzae (now known as Haemophilus influenzae) as well as strains of pneumococcus, streptococcus, staphylococcus, and Moraxella catarrhalis bacteria. These bacterial vaccines had no chance of stopping the pandemic which, we now know, was caused by a new strain of the influenza A virus.
Where are we now?
In the 100 years since the Spanish flu outbreak, there have been four influenza pandemics: 1957-1958, 1968-1969, 1977-1978, and 2009-2010. None were as lethal as the 1918 outbreak.
However, annual outbreaks of seasonal influenza cause between 290,000 and 650,000 deaths per year globally. The death rates are lower because (a) vaccines are available (b) healthcare and hygiene is vastly superior than conditions a century ago and (c) the viruses that cause seasonal flu are less dangerous – and less likely to be fatal to those infected.
Nonetheless, flu viruses can change from one year to the next. Experts continue to worry that a new flu virus could some day emerge with the potential to cause the kind of destruction seen in 1918.
The WHO is warning that low uptake of seasonal flu vaccines in Europe, is leaving vulnerable people at risk should an outbreak occur. Fewer than one third of older people are vaccinated in half of the 53 countries making up the WHO’s European region.
In fact, vaccination rates among high-risk groups have fallen in the years since the 2009-2010 pandemic.
‘Vaccination is the most effective measure to prevent severe disease caused by influenza. However, according to our research, influenza vaccination uptake has been steadily declining in a number of countries in the European Region,’ says Dr Zsuzsanna Jakab, WHO Regional Director for Europe. ‘This is of serious concern now for people at higher risk of severe consequences, especially older people, and in the future potentially for the entire population, as the production of pandemic vaccines is closely linked to seasonal vaccine use.’
In the EU, health ministers have set a target of vaccinating 75% of citizens in high-risk groups. With the exception of the UK and the Netherlands who have met this goal and are consistently above or close to the target, most EU countries are a long way from reaching their goal.
‘All European Union Member States have signed up to the goal of reaching 75% uptake among older people and other vulnerable groups; however, these targets are not being reached,’ says Dr Andrea Ammon, Director of European Centre for Disease Prevention and Control (ECDC).
As we prepare to mark the centenary of the worst flu pandemic in recorded history, it is time to step up efforts to improve flu vaccine uptake.
Older people at higher risk of death from influenza
The WHO estimates that over 44,000 people die annually of respiratory diseases associated with seasonal influenza in the WHO European Region, out of a total of up to 650,000 global deaths.
According to annual surveys for the ECDC and WHO, although 34,000 (over 75%) of these deaths in Europe are among people aged 65 years or above, vaccine uptake remains low in this group. Half the countries in the WHO European Region are vaccinating fewer than one in three older people.
As for the other at-risk groups:
- vaccination was generally recommended for people with chronic illnesses; however, coverage was below 40% in most countries;
- almost all countries recommended influenza vaccination for health-care workers, but the majority reported influenza vaccine uptake as being as low as 40%;
- in total, 90% of countries had vaccine recommendations for pregnant women in 2014/2015, compared with 40% before the 2009 A(H1N1) pandemic; however, coverage overall was low, with half the countries reporting uptake below 10%;
- fewer than half the countries, most of them in eastern Europe, recommended influenza vaccination for young children; vaccination coverage ranged from less than 1% to 80%.





Mary O Brien-Sheehan
May 2nd, 2018
Due to cotraversaries re: vaccine the % of the herd protection in the population falling year on year. Time to consider compulsory vaccination. Historically we are due a big whammy soon with antibiotic resistant strains-lethal outcome.
Kurt Standiford
April 1st, 2019
What if the Spanish flu was actually an Ebola like virus? The Spanish Flu had all the markings of a hemorrhagic outbreak, if not worse. It spread faster than a normal flu, killed quicker, especially younger people and lasted longer than any recent flu.
Jack
May 8th, 2019
The symptoms of ebola vs the symptoms of H1N1 influenza 1918 pandemic aren’t the same. Neither are the mortality rates. EBOLA ISN’T THAT VIRULENT. Spanish flu killed less than 4% of the worlds population, and about a quarter were affected. Compare that with the effects of an Ebola virus on a similar scale. Influenza has respiratory symptoms like sore throat and cough, but also body aches and fevers. Ebola has similar symptoms, but they are much worse.
At very least, influenza’s defining feature is its virulence, or ease of transmission. There has been ideas for horror dystopsian books where influenza experiences a genetic shift and is combined with, say, rabies. The idea behind this is that it could take on the potency of each, combining with influenza’s virulence.
Sorry about the rambling, but I suggest you research Ebola. They aren’t even related closely.
Jack
February 23rd, 2020
Whenever someone starts quoting statistics, or referencing sources or even worse, suggesting others do some research, FOX viewers get skip to the next comment.
Steve
March 14th, 2020
They exhumed dead soldiers from the permafrost in Alaska and found it was H1N1 with avian genes associated. Yes, it was a bird flu. Thus the global concern and monitoring of migratory birds with the concurrence of a flu of avian origin and H1N1.
Stefanie bond
March 22nd, 2020
I want to get rid of the shelter in place law and restore our freedom of choice. The law has to go
Gary Finnegan
March 23rd, 2020
What law are you referring to?
T Fowler
April 8th, 2020
This was written in 2018 🤭
joe
March 21st, 2020
antibiotics cannot treat flu which is a virus, do not need lectures from someone about mandatory vaccine who does not understand this simple fact.
Pingback
January 10th, 2020
[…] this, vaccination rates have astonishingly decreased since 2010, particularly among older groups that are more vulnerable to seasonal flu. This decrease in […]
Nicholas Hobart
March 20th, 2020
if only they knew what would happen in 2020
Pingback
January 10th, 2020
[…] this, vaccination rates have astonishingly decreased since 2010, particularly among older groups that are more vulnerable to seasonal flu. This decrease in […]
Patti Kanduch
February 9th, 2020
Ebola and spanish flu both bleed inside.
Shawn
February 14th, 2020
How’s those vaccines working out against Coronavirus? Just more liberal money grab, does not prevent anything. Makes people more sick. If you prevent against one disease another will take its place, and the more you fight them the worse you make them. Re:superbugs.
Gary Finnegan
February 14th, 2020
Dear Shawn, you are not correct about flu/Coronavirus. They are separate viruses. Flu is still circulating in areas where Coronavirus is present. Those who are vaccinated against flu are less likely to have flu. It has no impact on their risk of catching other viruses.
As it happens, several research efforts are under way to try to develop a Coronavirus vaccine. This will take some time – probably more than a year.
Regarding vaccines and superbugs, vaccines actually play a positive role in reducing antimicrobial resistance.
Jack
February 23rd, 2020
Gary, you don’t seem to know that flu=coronavirus. Step back, take a deep breath, and start over.
Gary Finnegan
February 24th, 2020
No, it’s not.
https://www.who.int/health-topics/coronavirus
Jack
February 23rd, 2020
Knuckle dragging, mouth breathing, climate denying, Trump voting MORON.
Kris Henri
March 3rd, 2020
https://www.hopkinsmedicine.org/health/conditions-and-diseases/coronavirus/coronavirus-disease-2019-vs-the-flu
John
March 11th, 2020
Feel better now Jack TV hat the mouth breathers were able to educate you?… Finally?
Flu is not coronavirus. Disregard the article’s comparisons.
Boghos L. Artinian MD
March 12th, 2020
The Corona pandemic has become a ‘Russian Roulette’ with a 3% chance of firing a bullet into one’s brain once the trigger is eventually pulled for every single person on the globe!
Peter Akinola
March 15th, 2020
On hindsight, you could say this article was quite prescient! Coronavirus is new mega pandemic with a relatively high death rate of 1.5 – 5%. It is interesting to see how measures to tackle such global scale pestilence have evolved since 1918.
Pingback
March 16th, 2020
[…] 100 YEARS AFTER ‘SPANISH FLU’: IS THE WORLD READY FOR THE NEXT PANDEMIC? (Posted October 24th, 2018) […]
Daniel Gant
March 20th, 2020
“Is the world ready for the next pandemic?” The answer is no. And the quicker we move to a total shutdown like China did. The quicker we can stop this spread.
Robert Cordell
March 27th, 2020
Daniel Gant – no! We need NOT to stop the spread. We just need to let it spread slowly enough to avoid overwhelming beds, respirators etc. The Covid ‘plague’ will end EITHER by vaccine creation (be so good) OR herd immunity. The latter depends on controlled spreading (albeit with consequential death), the former on time and scientific effort. I’m up for either but would prefer to avoid dying myself! BUT if we shut down world commerce and industry for too long, world consequences will be even worse.
Trump may sound mad, look mad and even be mad but his drive for ‘fast brakes off’ is right.
Marie A Birkbeck
September 4th, 2021
I for one do not need to lose several family members to this pandemic for the
anti-vaxxers to sit up and take notice
When ITF are people going to realize that all the measures put in place by CDC are being initiated for our own good and the good of the community in which we live
Me
April 8th, 2020
Do you all realise this was wrote 2yrs ago 🤔
Dr Shashwat Jain
April 21st, 2020
that’s amazing to see !!!!
James
April 26th, 2020
That’s why it’s so interesting. It shows that governments knew what to expect and did nothing to prepare for it!
Marie Annette Birkbeck
September 4th, 2021
who the heck cares? it is all still as relevant today as the day it was publihed
Narendra
April 14th, 2020
do we have vaccination for this Spanish flu?
Trickedgrayfox
March 21st, 2020
Nope, no we weren’t. “Sad!”
Robert Cordell
March 27th, 2020
Daniel Gant – no! We need NOT to stop the spread. We just need to let it spread slowly enough to avoid overwhelming beds, respirators etc. The Covid ‘plague’ will end EITHER by vaccine creation (be so good) OR herd immunity. The latter depends on controlled spreading (albeit with consequential death), the former on time and scientific effort. I’m up for either but would prefer to avoid dying myself! BUT if we shut down world commerce and industry for too long – doom.
Trump may sound mad, look mad and even be mad but his drive for ‘fast brakes off’ is right.
JK Kelly
March 29th, 2020
Virus is bad as is panic. Avoid both!
MAte
April 13th, 2020
Sadly we can now say we were not. COVID-19. The US for all it s greatness is now suffering due to its arrogance. A controlled reopening of the world will take place, cases will go up, new treatments will keeps deaths lower but not gone. This will continue until there is a vaccine or until antibody tests verify herd immunity. The next 12 months will be the most painful the world has ever seen. We were not ready, we responded poorly and we are 10 steps behind. 2019/2020 will become another part of a history book that again, no one will learn from ….sad.
Harinder singh
April 21st, 2020
Could we stop eating non veg and could human being reduce their dependence on animals for livelihood?
Could chna, south Asia countries ban their wet markets or stop dealing in trade of exotic animals. Could USA 🇺🇸 shutdown their supermarkets where red meat of beef, cow, lambs, chicken, goat’s, sea food is sold.
Jahar Chakraborty
April 24th, 2020
Yes everyone should be vegetarian
Coweater
May 3rd, 2020
No beef is good for health and there is no virus spread from beef
Harinder singh
April 21st, 2020
Could big pharmaceutical companies and virology and epidemiology Institute worldwide stop experimenting of vaccines made of bacteria, chemical toxic and animals body parts and then testing those vaccines on animals like rat 🐁, guinea pig🐷 etc
Marie A Birkbeck
September 4th, 2021
OH FFS take a reality pill!
Bethany
April 24th, 2020
God, I am sorry about how uninformed some people are. No matter how much research and stats you show them, they disregard it for YouTube sources , and political conspiracy theories.
However, in the chart with the two rates, was that the regular influenza vs the Spanish flu? Love the article.
Not an idiot
April 26th, 2020
Covid-19 isn’t a virus, it is an exosome.
Exosomes exist naturally in your body and protect cells against toxins. Exosomes can be released by cells to fight bacteria, a virus, or they can even be released when a person is experiencing extreme fear.
The “covid” test actually tests for the RNA in these exosomes, so there are people who aren’t even necessarily sick with anything who are positive. These people are the “asymptomatic covid-19” positive test results.
The purpose of this lie is to scare the entire world into taking a vaccine. Known eugenicist, Bill Gates, is spearheading this effort.
A small portion of the total number of vaccines will sterilize the people taking it. This will curb population growth, just as Bill Gates had said numerous times that we need to do- and he said we need to use vaccines to do it.
You may start to feel better that the world is about to start to reopen. Curb your enthusiasm, as just as they have programmed you in articles like this- the “virus” will be presented to have a massive comeback. It’s inevitable, as the test tests for a naturally occurring RNA in your body. The second time, the lockdown will be even more devastating. People will be begging to take a vaccine to end the world “crisis”.
Buckle up, folks. It’s about to get REALLY bad. The world is about to fall apart, all in the name of future population control.
John
April 26th, 2020
I just wrote a comprehensive explanation of this exosome testing that is being passed off as covid 19. It eased posted, and was deleted.
Thank you for confirming, vaccinestoday. If it wasn’t true, you wouldn’t have removed it.
Gary Finnegan
April 27th, 2020
Your post hasn’t been removed. It was submitted on a Sunday evening. We moderate external comments, according to our published guidelines, primarily to protect against libelous comments against individuals. Publication of a comment does not mean our Editorial Board agrees with the person who posted it.