It has been a miserable winter for Europe’s health services. Some called it a ‘tripledemic’, as influenza, RSV and COVID-19 put enormous pressure on hospitals across Europe. In addition, cases of pneumococcal disease and an uptick in other seasonal illnesses combined to increase demand for healthcare.
In France, a surge in patient numbers and a staffing crisis made the new-year period exceptionally challenging. Children’s hospitals in Spain, Sweden and Ireland saw unusually high numbers of young patients admitted. The situation mirrored challenges faced in the United States where some hospitals were overwhelmed in November.

The crisis was not unforeseen: doctors, scientists and politicians warned of the risks of a bad flu season this year, particularly after Australia was hit hard and early during its winter. Flu vaccine uptake in Europe is, in most countries, below target.
Throughout the year, experts also encouraged the public to keep up to date with their COVID-19 vaccines, including newly-developed omicron boosters. However, several countries reported much lower interest in COVID-19 jabs this year.
So what’s happening now?
Data from the European Centre for Disease Prevention & Control (ECDC) confirms that the flu season arrived months earlier than usual in the autumn. It also appeared that cases of flu were in decline until new data showed a slight uptick at the end of January (see infographic).
On occasion, flu seasons can have two peaks. Last year, the flu season had barely started at this time of year, so it would be unwise to declare victory so early in the season.
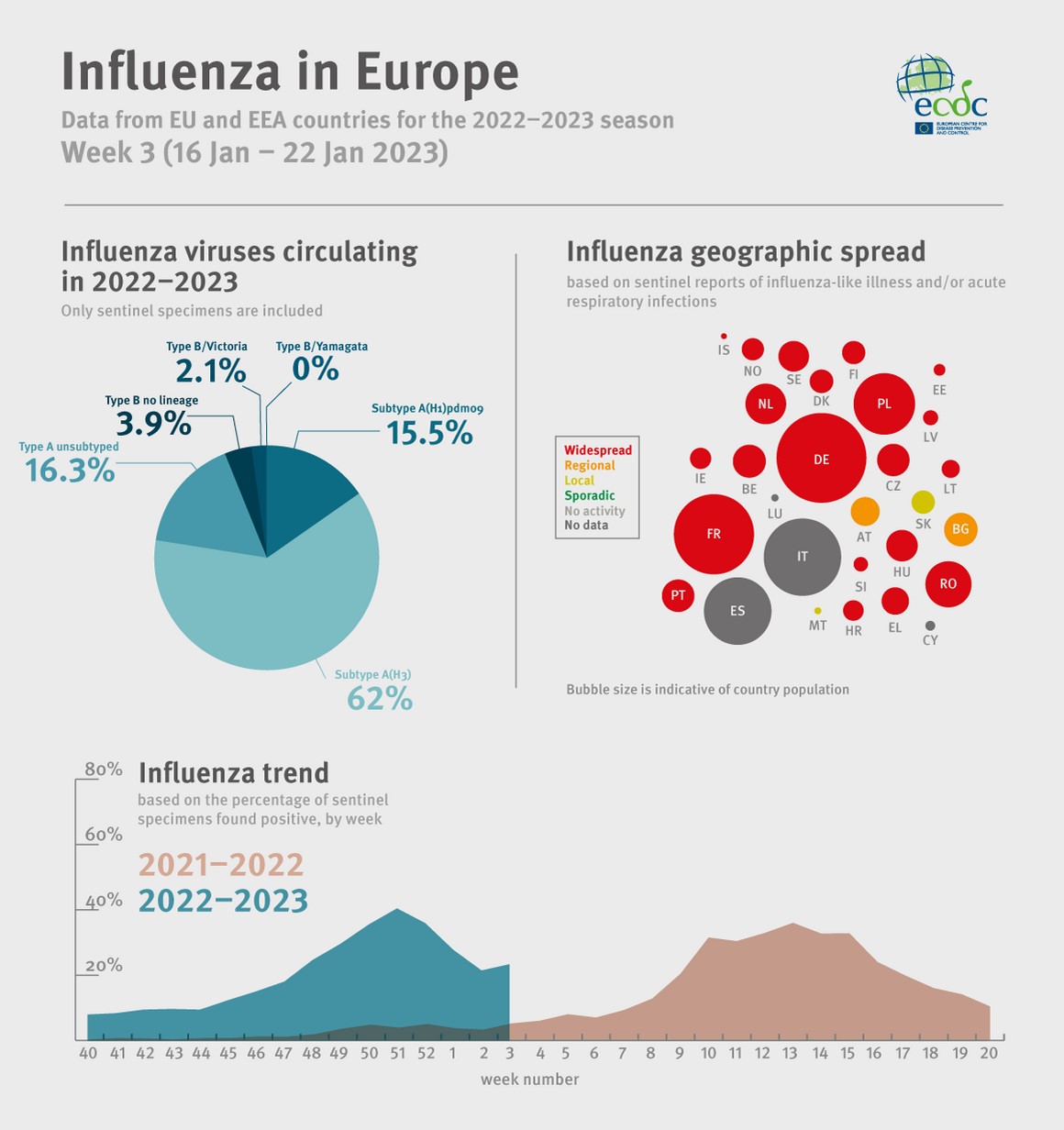
A sustained dip or plateau in case numbers would be a source of some relief to under-pressure hospitals. So too is the apparent easing of RSV cases which dominated the headlines in autumn and early winter.
The situation with COVID-19 is even less uncertain. Testing rates are much lower than last year, and gene sequencing, which can identify which variant of the virus is causing illness, has also declined sharply. However, the ECDC indicates that the overall burden of COVID-19 is improving, after a torrid holiday period.
COVID-19: The Kraken variant
There is one dark cloud on the horizon: the arrival of a new COVID-19 variant known as Omicron XBB.1.5 and sometimes referred to as Kraken.
As this variant is still relatively new, and there is less real-time data available than in earlier phases of the pandemic, experts are still working to determine whether it might be more transmissible. Crucially scientists are keen to know whether the new variant is better at evading the immune system.
Early indications are that the new version of SARS-CoV-2 is no more severe than previous versions. ‘There is no reason to think that XBB.1.5 is of any more concern than other variants that come and go in the ever-changing landscape of COVID19 mutants,’ according to Prof Andrew Polland, Director of the Oxford Vaccine Group at the University of Oxford.
The ECDC says Kraken has reached Europe but is still circulating only at ‘very low levels’. Its rapid growth elsewhere in the world suggests it will eventually become the dominant version of COVID-19.
‘In light of this, ECDC recommends carrying out appropriate testing and sequencing, increasing COVID-19 vaccination uptake, and reinforcing prevention and control measures,’ said. Andrea Ammon, ECDC Director. ‘Staying at home when ill, teleworking, good ventilation of indoor spaces and appropriate use of face masks should be considered.’
We may be approaching the tail end of a particularly rough winter in terms of respiratory viruses. The question now is what lessons can be learned for next winter.
Next autumn, when experts urge the public to have their vaccines, will people in Europe remember that hospitals were overwhelmed this year and roll up their sleeves? Will those who were nervous to attend emergency departments due to overcrowding, or whose hip replacements or colonoscopies were postponed make the link between vaccination and sustainable health systems?
Or will the memory fade, allow complacency to return once more?




