The European region has committed to eliminating viral hepatitis as a public health threat by 2030. This would significantly reduce rates of liver cancer. To succeed, high rates of hepatitis B vaccination are essential.
Belarus, Kyrgyzstan, Turkmenistan and Uzbekistan are the latest countries to reach their hepatitis B control targets. They join Georgia, Italy, the Netherlands, the Republic of Moldova and the United Kingdom on a list of nine countries to achieve the goals set out in the Action Plan drawn up by the WHO European Region.
The European Technical Advisory Group of Experts (ETAGE) adds countries to the list of nations where hepB is under control based on vaccination coverage, measures to prevent mother-to-child transmission, and evidence of falling hepatitis B rates. Other countries are likely to join the list in the coming years, but to achieve its goal, all 53 nations of the European Region will need to demonstrate that they are hitting their targets.
What is hepatitis?
There are several types of hepatitis (A, B, C, D & E) which cause a range of liver problems. Hepatitis A, B and C are more common than D and E.
Hepatitis A is associated with poor food hygiene practices. Outbreaks of hepatitis A are not common in Europe, but hundreds are recorded every year. The associated illness is usually relatively short, compared to the impact of hepatitis B and C which cause long-term health problems.
Hepatitis A can be controlled through a combination of better hygiene and hand-washing, as well as vaccination. The first hepA vaccine was approved in Europe in 1991, although it is not widely recommended in the Region.
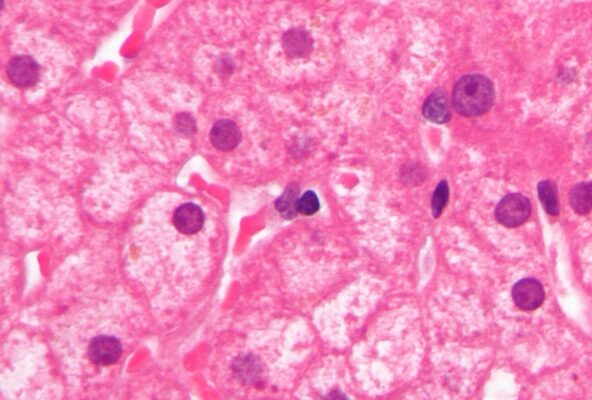
Hepatitis B can cause serious liver damage (cirrhosis) and liver cancer. It can spread from mother to child and sometimes between young children. The disease affects 14 million people in the WHO European Region.

Vaccines will play a key role in controlling hepatitis B, a life-threatening viral illness The vaccine is estimated to be 95% effective and universal hepB immunisation programmes have been introduced across Europe.
The first hepB vaccine was developed in the 1980s. The WHO advised in 1993 that all countries include hepB vaccines in their universal schedules. 190 countries now include the vaccine in their schedules. Cases have been trending downwards in the EU in recent years according to ECDC data.
There is no vaccine against hepatitis C, a viral illness spread through contact with the blood of an infected person. The most common way to contract hepatitis C is through sharing needles used for injected drugs. Unlike hepatitis B for which there is no dedicated therapy, antiviral medications can be used to treat hepatitis C. These safe and effective therapies cure more than 90% of infected patients within 8 to 12 weeks.
Preventing infection, controlling cancer
‘As more countries reach the regional targets set for hepatitis B control, their efforts collectively bring the Region closer to achieving the ultimate goal of eliminating viral hepatitis as a public health threat by 2030,’ according to the WHO Regional Office for Europe.
Reducing rates of liver cancer through hepatitis B vaccination is among the goals of the EU Beating Cancer Plan. This action is supported by patient advocates, notably the European Liver Patient Association (ELPA), which is urging authorities to ensure high and equitable uptake of the vaccine.
ELPA calls for the EU and all Member States to take immediate action to strive to overcome the low and inequitable HBV vaccine uptake for all ages, eventually translating this into reducing the burden of liver cancer. #EuropeanImmunizationWeek @EU_Health @AleksanderKrag pic.twitter.com/j8y4URmju4
— ELPA 🇪🇺🇺🇳 (@EuropeLiver) April 24, 2023



