My name is Davy Cotting.
I want to share the incredible story of my wife, Anaïs. We’ve shared our lives for 13 years. Our daughter, Chloé, is now four years old. We live in a small countryside village in France.

One year ago, at the age of 35, Anaïs was in excellent health. She had no known illness or comorbidity and was not receiving specific medical treatment.
She had worked as a healthcare assistant for several years. A few days after her night shift at the hospital, on Sunday evening, March 5th 2023, Anaïs started to have a headache.
On Monday, March 6th, she consulted her doctor, who diagnosed her with a flu-like illness. The initial symptoms didn’t seem alarming: just a flu-like condition accompanied by slight fatigue, a cough, and a mild fever.
On March 8th, I dropped our daughter — who had also fallen ill — at her grandmother’s so that my wife could rest. Later, Anaïs, tired, went to bed. At 9:20 PM, she woke to tell me she was feeling really unwell and wanted to sleep downstairs on the couch.
I found a bloodstain in the bedroom and immediately went downstairs and asked my wife where the blood came from. She said ‘Yes,’ and that she was also having difficulty breathing and felt chest pain.
I called the emergency medical service immediately and was advised to consult an on-call general practitioner, located in the hospital where Anaïs worked. They also asked if I could drive my wife myself.
At the clinic, the doctor, alarmed by her state, measured her oxygen saturation (SpO2). He was very surprised by the result of 80%. A normal SpO2 level ranges between 95% and 100%. Such a low SpO2 level, indicating a very low oxygen in the blood, requires urgent medical intervention.
He called the emergency medical service requesting an urgent ambulance with oxygen or a Mobile Intensive Care Unit (SMUR) and an ambulance with an oxygen bottle was dispatched.
When the paramedics arrived, approximately 20 minutes later, they used an oxygen saturation monitor, which indicated 72%. They administered oxygen and immediately transferred her to Emile Muller Mulhouse Hospital – a larger hospital equipped with an emergency and medical resuscitation department.
‘Prepare for the worst’
At 11:12 PM, Anaïs arrived in the resuscitation area, and I waited anxiously in the waiting room, overwhelmed by stress.
At midnight, two doctors came to get me and quickly asked me a series of questions: ‘Have you been travelling? Is she taking any medications? Do you know of any allergies? Does she have any medical history? Any recent surgeries?’
I responded negatively to all these questions. That’s when they informed me about her critical condition.
I was in shock.
The doctors allowed me to enter the resuscitation area, where there were eight nurses and doctors around her. I was able to spend 10 minutes by my wife’s side. She was in total distress, panicked. Her gaze seemed to say, ‘I love you, take care of our daughter Chloé,’. She couldn’t speak anymore, she was choking and struggling to breathe.
They decided to proceed urgently with intubation. I immediately gave my consent.
At 05:42 AM on March 9th, at, a doctor took me to my wife’s cubicle. I was shocked to see her on a ventilator, with a tube in her mouth, and numerous cables connected to automatic syringe pumps going directly into her artery in her neck as well as a ventilator assisting her breathing.
The anaesthetist warned me, saying, ‘You can talk to her; you never know if patients can hear or not…’
Then the doctor said to me: ‘Sir, do you know what total organ failure is?’
I replied yes, and I burst into tears….
He continued,
‘We, unfortunately, have reached that point. Her heart is beating at 138 beats per minute and is trying to compensate for the lack of oxygen; it’s a real marathon for a person of her age and we hope the heart holds up. Regarding the lungs, the scan shows an image as white as yoghurt; there is no visible lung function; it’s filled with mucus, and we don’t know if we’ll be able to restore lung function. The kidneys have failed… we’ve put her on dialysis. Go home and prepare yourself seriously for a death. Within 48 hours, we’ll have a clearer picture.’
I was frozen, completely paralyzed by emotions.
At 9:42 AM, I was told that her condition was unstable, and they had to urgently place her on Extracorporeal Membrane Oxygenation (ECMO) – a critical medical intervention used when the vital functions of the heart or lungs are severely compromised. It is often employed as a last resort.

Tests confirm flu infection
Blood tests revealed Influenza A. Additionally, white blood cells and platelets were almost absent. Faced with this data, the doctors’ prognosis became alarming: ‘We feel like she’s slipping away from us.’
The following day, March 10th, I was informed of necrosis in the extremities of the hands and feet due to septic shock. Her foot was black at the extremities and purple up to the knee, while her fingers were also blackening at their tips, and her hand took on a bluish hue.
On March 17th, Anaïs faced severe complications including two collapsed lungs and a pleural effusion that needed to be drained.
On March 28th. Anaïs woke up but couldn’t speak. We communicated through eye blinks: one blink for ‘yes,’ two blinks for ‘no.’ She was very stressed and frightened, understanding the gravity of the situation. She saw her hands and quickly understood that there would be irreversible consequences.
‘A waking nightmare’
I spoke to her, tried to reassure her. On one hand, I was happy to see her awake but on the other hand, terrified at the thought that her feet were also black. Her blood pressure was already very high, and she clearly couldn’t express her fears and feelings.
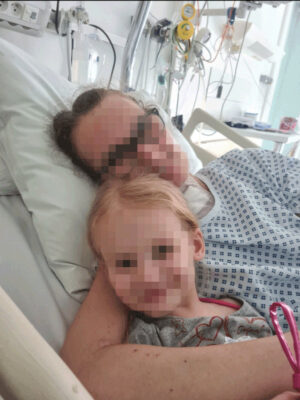
On March 30th, the medical team asked for my agreement to perform a tracheostomy, to promote breathing and attempt to wean her off the ECMO. On April 3rd she developed a fever and experienced the worst life-threatening complication: ‘a superinfection under ECMO.’
I was told that the chances of recovery were clearly very slim, and the doctors had not yet identified the microorganism responsible.
The team decided to perform prone positioning, requiring the intervention of eight people for about an hour.
Ultimately, the repositioning worked.
Anaïs was awakened for the third time on April 16th. On April 17th, the ECMO was finally removed. Simultaneously, they would attempt to reduce dialysis to assess kidney function.
However, this improvement was short-lived. On April 19th, Anaïs experienced a powerful allergic reaction.
Anaïs was in intense pain. Although awake, the pain prevented her from communicating.
She could see but couldn’t move; she could hear but couldn’t respond. She was a prisoner of her condition.
I didn’t dare even imagine how long the days were for her and what she might be thinking.
The fear and the risk of a setback were very present for me as well as for the medical staff.
On April 27, Anaïs woke up, conscious and without pain. Although she couldn’t speak, she managed to write on a tablet despite the necrosis in her fingers. Her first words written on the tablet were: ‘I’m thirsty, I want to drink’, ‘I love you, how is Chloé?’. I was also able bring her mobile phone so we could communicate whenever she wished.
The next day, a vascular surgeon informed her of a plan to amputate her feet at the level of the 1st metatarsal, as well as four phalanges in her hands. This news plunged her into intense depression, questioning the meaning of her survival.
I felt completely overwhelmed, powerless, and saddened. I didn’t know what to say or how to help her regain her spirits. I understood that she needed time to process this news and come to terms with the situation.
Hearing her voice again
On May 4th, there was a significant improvement in Anaïs’s overall condition. She almost no longer needed oxygen. Her previously unstable blood pressure was improving. Doctors stopped dialysis, as her kidneys gradually resumed their functions.
A nurse placed a new tracheostomy tube and I finally heard my wife’s voice again. She was gradually regaining her memory and she could begin to eat by herself.
Her condition continued to improve gradually, and the tracheostomy tube was removed on May 14th. On May 15th, Anaïs left the intensive care unit. The entire unit paid tribute to her with a guard of honour naming her ‘Miraculous Phoenix’ due to her remarkable recovery.
Anaïs spent 69 days in the medical resuscitation care unit where she narrowly escaped death several times, including:
- 61 days on a ventilator
- 57 days on continuous dialysis
- 40 days on ECMO
On May 20th, our daughter Chloé was finally able to see her mom after more than two and a half months of separation. On June 1st, surgeons amputated both feet at the 1st metatarsal level and four finger phalanges (the thumb, index, and ring fingers on the left side, and the little finger on the right side).
On June 22nd, a second surgical intervention was needed to remove a piece of excess bone from her left foot. The left foot’s ankle remained frozen.
The surgeon proposed a third amputation: ‘If we leave the foot as it is, you won’t be able to walk. If we perform an amputation 10 cm below the knee, you’ll be able to use a prosthesis and regain the ability to walk.’ The decision was heartbreaking but necessary. On July 15th, Anaïs underwent this third amputation.
On August 2nd, our daughter celebrated her 4th birthday, and we celebrated together at the hospital.
On August 10th, Anaïs was transferred to the rehabilitation service.
Rehabilitation: a long road
Anaïs has shown incredible determination to regain her mobility and resume a normal life during her rehabilitation. From the very first day, she started using a wheelchair. A week later, she progressed to walking with prostheses and parallel bars. Two weeks afterward, she managed to walk with crutches. And two weeks after that, Anais succeeded in walking with just crutches. Currently, Anais can even walk a short distance without any assistance.
Anaïs is still confronted with a significant pulmonary handicap, which exhausts her considerably during prolonged efforts.

On my birthday on September 16th, at 9:00 in the morning, the doorbell rang, and I found my wife standing outside. It was and will forever be the most beautiful birthday surprise. I cried tears of joy.

On December 22, 2023, Anaïs returned home. Her fight for life, her love for Chloé and me brought us together. We aspire to regain a ‘normal’ life despite the challenges associated with disability and the significant upheavals within our family. However, she will need regular visits from a home nurse and will have to go to the hospital three times a week to continue her rehabilitation.
My life has been deeply disrupted and emotionally challenging. Apart from the very frequent hospital visits, I took sole responsibility for taking care of our daughter Chloé during the long months at the hospital, while she deeply felt her mother’s absence during that period.
I lost my job after six months. The psychological impact and anxiety have had a profound impact on me. My wife has also realised that she won’t be able to continue her career as a nursing assistant as before.
We have to rethink our housing situation as our house is built on two levels and we will need to adapt it and will need to replace our car.
Why we are sharing our story
We are sharing our story because we don’t want this to happen to anyone else. It can happen to anyone, so we want to share the following.
- Vaccination remains the only effective protection against flu viruses.
- Changing the perspective on flu vaccination is crucial. Flu is not just a cold; it can be deadly, not only among the elderly or fragile individuals.
- The impact of a disability on life is enormous An accident or illness may not give a warning.
- Sharing our experience is also a way to remind people of how precious life is. It’s essential to enjoy it fully because we never know how or when it will end.
- Finding Support: If you wish to support Anaïs in her battle to improve her daily life, I have set up a foundation.
Beyond the financial aspect, your contribution will also provide her with psychological support by showing her that she is surrounded and supported by a large number of people. You can also leave a message of support for Anaïs by sending an email to aideanais@email.fr. Your words of encouragement will be greatly appreciated.
A huge THANK YOU to all healthcare professionals who, through their dedication, commitment, and expertise, work every day for everyone’s well-being and health. Your determination and compassion make all the difference. We are immensely grateful for your support and your invaluable work. And especially to the staff at GHRMSA.





