Every year, influenza immunisation campaigns encourage health workers to be vaccinated. The messages are clear: people working in hospitals and nursing homes are at higher risk of exposure to flu viruses.
If that’s not enough, staff are reminded that unvaccinated health professionals could infect vulnerable patients with the disease. And that an outbreak among nursing and medical teams would leave services stretched at a high-pressure period of the year.
Health workers are also key advocates of vaccination, regularly interacting with people in risk groups – pregnant women, older people, patients with chronic conditions – and some staff are responsible for administering vaccination.
For health workers, the flu vaccine is free, usually available at the workplace, and staff are targeted with annual reminders.
With so many good reasons to vaccinate, you might expect vaccine uptake among healthcare workers to be exemplary. Unfortunately, it is not. In many European hospitals, staff vaccination rates are well below 50%.
This is sparked some debate about how to increase vaccination rates. Many US hospitals have made vaccination a condition of employment while Finland recently obliged healthcare providers (hospitals and care homes) to protect patients from vaccine-preventable illnesses – a move viewed as a heavy nudge towards vaccination.
National uptake among hospital staff in Ireland was around 45% last year, prompting the Royal College of Physicians in Ireland to call for mandatory flu immunisation for frontline healthcare staff.
Most European countries prefer persuasion but, despite an annual push for better flu vaccination rates, uptake has been stubbornly slow to improve.
Social marketing project
An innovative project in the west of Ireland tried something new. Around 15% of healthcare workers at hospitals in the region were vaccinated against flu when a social marketing expert and a public health specialist joined forces in 2016. The rate was particularly low among nurses at just 8.7%.
Dr Christine Domegan, Senior Lecturer at the National University of Ireland, Galway, matched her marketing know-how with the public health expertise of Dr Aine McNamara, Consultant in Public Health Medicine. Working with systems change experts, Dr Patricia McHugh and Dr Christine Fitzgerald, and Dr Katherine Harkin and Dr Diarmuid O’Donovan, they set out to understand why vaccine uptake was low – and to do something about it.
Together, the team devised an award-winning intervention, drawing on insights from the WHO’s TIP FLU project – a flu-specific version of the Tailoring Immunization Programmes approach. TIP focuses on identifying barriers to immunisation and understanding what makes people vaccinate – or not.
These principles have previously been tested in Lithuanian to improve flu uptake during pregnancy, in London to address vaccination rates in orthodox Jewish communities, and in several other settings.
The west of Ireland project included a literature review, a survey of attitudes, research on perceptions of immunisation, and interviews with nurses which fed into a Dynamic Systems Analysis.
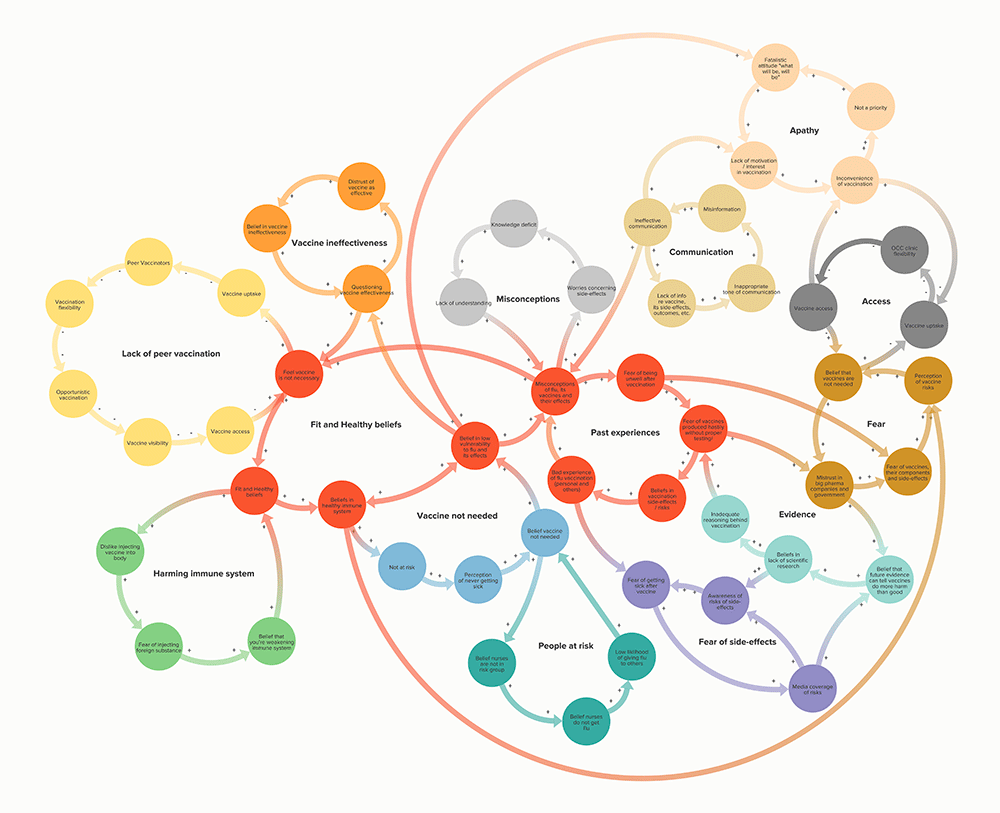
The survey, observations and interviews revealed that nurses were likely to believe that they are fit and healthy which, in some cases, led to the conclusion that vaccination was unnecessary. It also showed a lack of confidence in vaccine effectiveness and a belief among some that their immune systems would be strong enough to fight the flu virus. (In fact, healthy middle-aged people are among the hardest hit by the H1N1 strain of the flu which is circulating this season.)
There was another factor that is tricky to overturn in a flu awareness poster: apathy. Some nurses felt that even if they were to get the flu, it might not be serious and, in any case, they tended to be fatalistic – ‘what will be will be’, as one respondent put it.
Past experiences and anecdotes also played a role. Some had heightened concerns about side effects, possibly linked to media coverage, while others had a wider mistrust of government and the pharmaceutical industry.
 Dr. Áine McNamara, public health specialist, receives her annual flu vaccine from a peer vaccinator
Dr. Áine McNamara, public health specialist, receives her annual flu vaccine from a peer vaccinator
Solutions
The researchers identified a number of social marketing initiatives to address barriers to uptake. Peer vaccination was found to be an area with potential to turn the tide on nurse’s immunisation rates.
Peer vaccinators are nursing staff who administer the vaccine to their colleagues in the workplace. ‘They help by providing access, but they are also important as channels of information and communication,’ said Dr Domegan. ‘They deliver the educational component, build trust and answer questions.’
Peer vaccinators can also be influenza vaccination champions, but a range of champions can be recruited from different categories of staff within the hospital system, as well as outside of it, to serve as ambassadors for vaccination. ‘Flu champions’ could amplify the positive impact of peer vaccination, sparking a trend whereby vaccination becomes the norm on hospital wards.
Win-win
Emphasising mutuality – i.e. that flu vaccination is a win-win for nurses, their family and friends – was seen as more effective than taking a moralistic tone which tended to prompt resistance from some.
‘Social marketing is dependent on voluntary behaviour change,’ said Dr Domegan. ‘When we talked to different stakeholders it was common to hear, ‘if you’re a doctor or a nurse you should get the flu vaccine, it’s part of your job and it’s for the sake of your patients’. That’s a strong moral stance and some people see it that way, but there was a cohort that didn’t want to be told they had to do it on those terms.’
Flu literacy, combining science and statistics with scripts and storytelling, helped to deepen understanding of flu viruses, vaccines and the immune system. Communication approaches were tailored to the hospital size, as researchers found that different messages would be needed for small and large hospitals.
The team also sought to reframe influenza. Instead of associating ‘flu’ with colds and other minor illnesses, using the term ‘influenza’ can shift how people think and feel about the disease. ‘There are times when people trivialize the ‘flu’, so there are times when you need to use the word influenza to frame and underline the seriousness of it,’ explains Dr Domegan.
Using the insights provided by the project, Dr Domegan and Dr McNamara and colleagues guided hospitals to introduce targeted changes that helped boost average immunization rates. In the first year, vaccination rates rose from 15% to 25%; by the end of the second, they had more than doubled to 37%.
The project manager for the initiative became a strong flu champion and helped ensure the top-level management buy-in required to roll out the initiative.
The project won an award at the European Social Marketing Conference and continues in the west of Ireland. Research is now under way regarding flu vaccination uptake among nursing home staff, shifting the emphasis from a hospital to a community setting.
The Guide to Tailored Immunization Programmes (TIP)
TIP FLU Maternal Influenza Immunization
TIP FLU Health Workers in Montenegro




