Last year, 83% of the 3,616 measles cases reported in the EU were completely unvaccinated. The WHO – and, in all likelihood, your doctor – recommends two doses of measles vaccine.
Check your vaccine schedule here
In the wake of the death of a one and a half year old boy in Berlin, experts and health officials are crying out for action against outbreaks of this preventable and potentially lethal disease.
Germany has been dealing with a major outbreak since late last year and several other European countries have also reported epidemics.
Age discrimination?
Measles vaccines are part of childhood immunisation schedules so that we are all protected as soon as possible and for as long as possible.
But the disease can infect anyone. On average 40% of measles cases in the EU in the past decade were in people over 14 years of age.
Anyone who has not been vaccinated is at particular risk of infection, including adolescents and young adults who may have missed out on vaccination as children. However, it’s never too late to have the vaccine.
Children under one-year-old accounted for 6.2% of measles cases. These children are too young to have the vaccine and rely on the rest of us to stop the disease from spreading by vaccinating.
Scroll down for a video explaining herd immunity
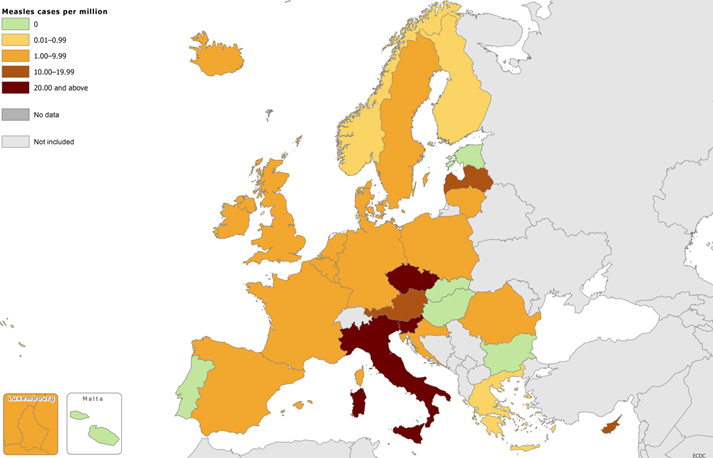
This graph of data from December 2014 (courtesy of the ECDC) shows the number of measles cases per million in EU countries.
You can see that Germany is not even the worst hit and that we might expect to be reading headlines about Italy, Slovenia and the Czech Republic if the disease is not contained there very soon.
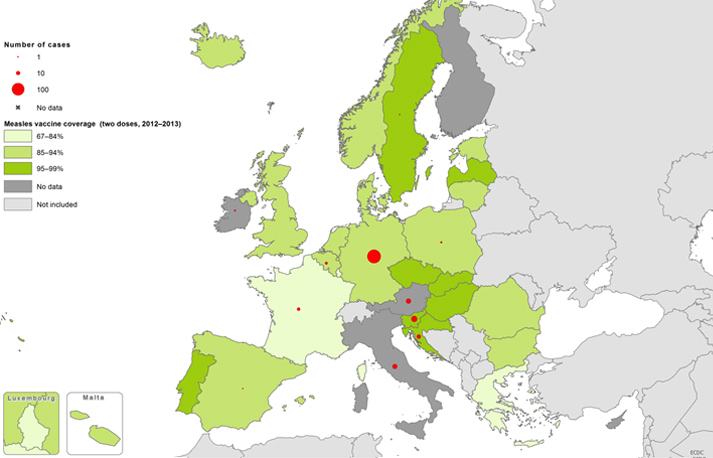
Here we can see vaccination rates in the EU in December 2014. The data for Italy is missing (i.e. the ECDC didn’t have it when creating this map last month).
One thing worth explaining is the relatively high vaccination rates in Germany at a time when they are suffering an outbreak in their capital city.
The trouble here arises from ‘clustering’. Yes, the overall average vaccine rates look reasonably good. But those who are unvaccinated seem to be clustering together in certain social groups or locations.
For example, a previous measles outbreak in Germany took off when it reached an anthroposophic school in Berlin where the proportion of unvaccinated people was much higher than in the rest of the country.
On other occasions, outbreaks can be centred on disadvantaged groups, such as the Roma communities, where access to health services or trust in authorities is low.
In both examples, ‘herd immunity’ has broken down. As this video explains, the virus finds it easy to locate a new unprotected person to infect and it just keeps spreading.
As the animation explains, if 95% of people are vaccinated, the disease has nowhere to go.
The situation in Europe is serious. The WHO’s regional office for Europe publicly called on ‘policymakers, health workers and parents’ to immediately step up vaccination as a target of eliminating measles this year looks increasingly unlikely.
For its part, the European Centre for Disease Prevention and Control (ECDC) says decades of progress are on the line if epidemics get out of control.



