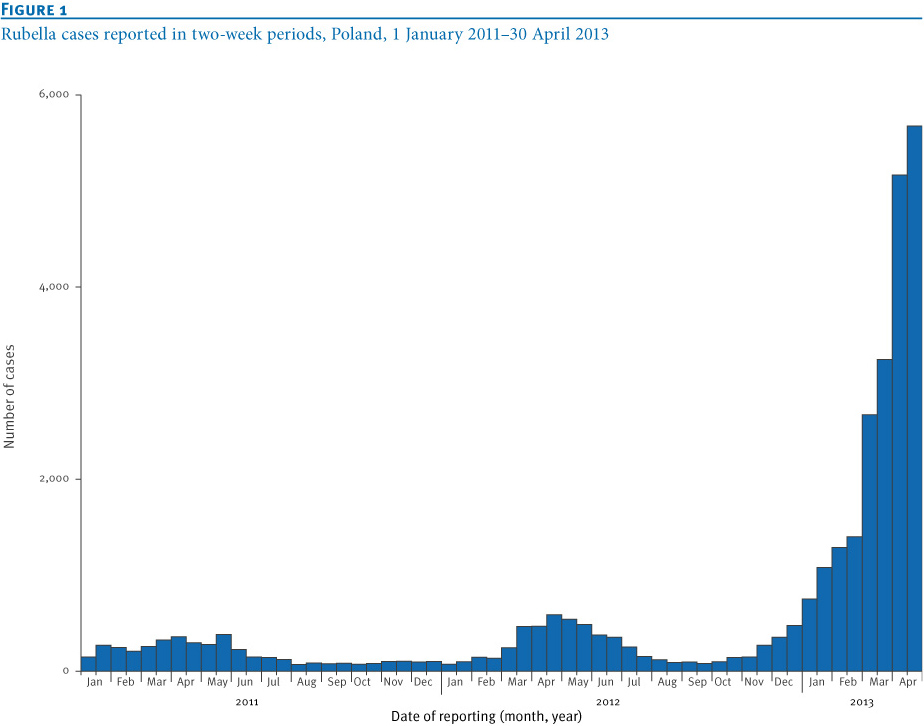
 Take a look at this graph from a recent paper published in the Eurosurveillance journal. It shows the surge in the number of rubella cases in Poland which began at the turn of the year and exploded in the spring.
Take a look at this graph from a recent paper published in the Eurosurveillance journal. It shows the surge in the number of rubella cases in Poland which began at the turn of the year and exploded in the spring.
The scale of the outbreak is so severe that the US has issued a travel warning to pregnant women traveling in Poland. The reason pregnant women are of particular concern also explains, in a roundabout way, why men are bearing the brunt of the current epidemic.
Rubella is usually a mild childhood disease but can cause serious birth defects if pregnant women are infected.
In addition to increasing the risk of miscarriage or still birth, infection with rubella during early pregnancy can result in Congenital Rubella Syndrome (CRS), in which the normal development of several of the baby’s organs is disrupted. The result can be anything from deafness and cataracts to heart problems and mental retardation.
Birth defects are found in as many as 85 of 100 babies born to mothers who had rubella in the first three months of pregnancy.
The potential for catastrophic defects caused by CRS led many countries, including Poland, to target young girls with the rubella vaccine when it was first introduced. In Poland, rubella vaccination was introduced in 1989 with a campaign focusing on 13-year-old girls.
In 2004, Poland began offering the combined measles, mumps and rubella (MMR) vaccine to boys and girls at 13-15 months of age, with a second dose at 10 years of age.
This means that most children old enough to be vaccinated are protected; most women of child-bearing age are protected; but there is a group of young men who are at risk.
A similar pattern was seen in Romania where an outbreak of more than 20,000 rubella cases was recorded in 2011-2012. Epidemics in Greece in 1993 and 1999 followed a similar pattern: a spike in cases among men, who had not been included in rubella immunisation campaigns, leading to a rise in cases among women.
Community immunity
Most young men will shake off rubella without suffering any lasting damage. The real problem is that young men are frequently in close contact with young women.
And even though uptake rates were reportedly high among women vaccinated during the era of the girls-only rubella campaign, there are always cases where girls did not receive the vaccine or where the vaccine did not work.
With rubella circulating in the community, the herd immunity that protected young women from exposure to the virus is gone. In short, young women need young men to be immunised.
Warning signs
The real tragedy of the outbreak in Poland and the inevitable birth of even a small number of babies with CRS is that it was predictable. Indeed it was predicted.
In 2011, experts from the World Health Organisation (WHO) identified a rubella immunity gap among adolescent males and young adults in Poland. They recommended additional immunisation of all adolescents and young adults specifically because rising circulation of the virus increases the risk of CRS.
According to a paper by scientists from Poland, Norway and Sweden, an “emergency catch-up” immunisation campaign is required to vaccinate young men who missed out, as well as a greater efforts to ensure that women of child-bearing age are immune to the virus.
They warn that Poland will not reach its targets agreed under the Europe-wide effort to eliminate measles and rubella by 2015.
Polish health authorities are now grappling with a serious public health crisis but other European countries with large cohorts of susceptible individuals have a chance to prevent rubella epidemics by taking the advice given to Poland two years ago.




