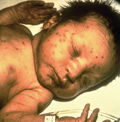
 Rubella – sometimes called German measles – is usually a mild childhood disease, but experts are deeply concerned by the serious birth defects it can cause if pregnant women are infected.
Rubella – sometimes called German measles – is usually a mild childhood disease, but experts are deeply concerned by the serious birth defects it can cause if pregnant women are infected.
In addition to increasing the risk of miscarriage or still birth, infection with rubella during early pregnancy can result in Congenital Rubella Syndrome (CRS), in which the normal development of several of the baby’s organs is disrupted.
The result can be anything from deafness and cataracts to heart problems and mental retardation.
Dr Nedret Emiroglu, Deputy Director of Communicable Diseases at WHO Europe, said CRS is very serious but preventable through vaccination.
Speaking to Vaccines Today after a conference on rubella elimination in Rome, Dr Emiroglu said a major rubella outbreak in Romania last year – with most cases recorded in unvaccinated adolescents – has added an additional sense of urgency to the elimination effort.
Ongoing efforts to eliminate measles in Europe by 2015 have had a major positive impact on the number of children affected by CRS. “Measles and rubella protection can be provided in a single vaccine so we can hope that both diseases will become a thing of the past,” Dr Emiroglu said.
One continent, many stories
When it comes to beating rubella, Europe is far from uniform in its approach. Each country has its own tale to tell, some with happier endings than others.
While Romania has been dealing with a major outbreak, Denmark, Finland, Sweden and Norway have recorded barely a handful of cases over the past five years.
The World Health Organisation is now setting up a formal expert group to verify whether Scandinavia can be declared ‘rubella free’.
But the divide is not just between north and south. Western European countries began incorporating the measles/rubella vaccines into the childhood immunisation schedule long before their Eastern European counterparts.
Until 2009, several countries in the 53-member region covered by WHO Europe were targeting their rubella immunisation efforts at adolescent girls and women of child-bearing age. Now though, all babies – boys and girls – receive two doses of the vaccine as a routine part of their immunisation programmes.
A collective effort
Wiping out rubella in Europe will require several strands of public health policy to come together, according to Dr Emiroglu. At the Rome conference, the International Pediatric Association – a leading group of experts in child health – committed to taking the lead in eliminating rubella globally.
This is essential, according to experts, as doctors have an important role to play in discussing immunisation with parents. “Paediatricians see the misery resulting from incomplete immunisation,” said Andreas Constantopoulos, president of the European Paediatric Association and president-elect of the International Pediatric Association.
Also crucial to success is beefing up disease surveillance systems. This means getting more accurate information on precisely how many cases of rubella there are and where they have occurred. (The Scandinavian countries have been particularly strong on this front.)
In the end, the fate of European efforts to defeat rubella lies in the capacity of millions of individuals to act in their own best interests and those of their neighbours.
Or, as Dr Nedret Emirolgu put it: “If the number of people protected against rubella is too low, it puts people at risk – particularly those who cannot be vaccinated for health reasons. It’s a matter of collective responsibility.”
The following is a transcript of our interview with Dr Nedret Emiroglu, Deputy Director of Communicable Diseases at the Regional Office of WHO for Europe
Vaccines Today: Tell us about the recent meeting in Rome which focused on rubella elimination.
Nedret Emiroglu: We had good technical discussions about what needs to be done in Europe and reviewed what has been done elsewhere, particularly in the Americas. One outcome was that International Paediatric Association said it would like to lead globally. This is significant because engaging paediatricians is going to be important if we are to reach our target of eliminating rubella.
VT: One of things the conference looked at was rubella-related birth defects. What kind of complications can arise from rubella infection during pregnancy?
NE: Rubella is seen as a mild childhood disease in most cases. The problem is that the public is taking it too lightly even though we see complications such as encephalitis and there can be rare fatal complications. It becomes more important if acquired during pregnancy especially during first trimester. Rubella infection can cause miscarriage or still birth, or delivering baby with CRS [congenital rubella syndrome].
Problems arising from CRS are mostly related to anatomic changes resulting from interference with organ development in early in utero development. For example, babies could be born with cataracts, deafness, CVS [cardio-vascular system] problems, CNS [central nervous system] disorders, mental retardation, autism and so on. Then we could also see hepatic [liver] or splenic changes. Late manifestations like diabetes are also possible. CRS is very serious but preventable.
VT: When should women be vaccinated?
NE: There are two strategies, both aiming to ensure that all women of child-bearing age are immunised: either babies are immunised in early childhood or adolescents and women of child-bearing age can be targeted. In Europe, since 2009, all 53 members of the WHO Europe region are giving two-doses of rubella vaccine as part of childhood immunisation programmes. This means that from now on all children are vaccinated, including baby boys.
VT: What is the connection between measles elimination and rubella elimination?
NE: In the European region we have set measles elimination as an important goal. The target date is 2015 and this has been endorsed at highest level by delegations from 53 member states. Measles and rubella protection can be provided in a single vaccine so we can hope that both diseases will become a thing of the past.
It is efficient, practical and feasible to eliminate rubella at the same time as measles. It can be a mild disease in most cases but CRS has very serious consequences. I’m very pro-vaccine and don’t want anyone to get a preventable disease.
Theoretically measles and rubella should be eliminated around the same time. Western Europe started immunising against measles/rubella together earlier than some in Eastern countries of the European region.
Elimination requires a high level of immunisation coverage – two doses for all babies. For measles we need at least 95% coverage at the local level so there are no susceptible pockets. Rubella requires a lower level to achieve herd immunity as it’s less infectious. The threshold is around 80%.
VT: How common is rubella in Europe?
NE: Surveillance is something we need to support countries with as it plays a critical role. Unfortunately rubella surveillance is not as strong as measles surveillance. Suboptimal surveillance means we don’t have the full picture. The numbers officially reported to WHO in 2007 show there were 68,000 rubella cases. This decreased to 10,500 in 2010 but there was a huge outbreak in Romania in 2011.
VT: Measles numbers have been high in Roma populations, particularly in Bulgaria. Is this hard-to-reach group recording a higher level of rubella cases?
This rubella outbreak was very much linked to the Roma population. There is an accumulation of people who were never immunised so we’re seeing it on older age groups as well as in children.
VT: Why has rubella been eliminated in some developed countries but not all?
NE: They had a campaign approach in the US. Perception in the US is that one-time campaigns are more acceptable, whereas in Europe we tend to go for immunisation service delivery through routine immunisation. Campaigns were never that popular in western parts of the region. The political commitment was there [in the US], plus they committed the resources, and rolled out a strategy that worked for their region.
VT: What can be done to eliminate rubella in Europe and who is responsible for achieving this? Is there a deadline or target for elimination?
NE: The WHO is a global health leader. We are responsible for looking at what’s feasible and overcoming difficulties that particular countries face. This is the responsibility of the WHO. Ultimate ownership and responsibility for immunisation programmes rests with member states.
VT: What message can be sent to people reluctant to be vaccinated or complacent about rubella?
NE: Individuals have rights and responsibilities. If you’re not immune it’s not just your personal issue, you’re posing a risk to others. If the number of people protected against rubella is too low, it puts people at risk – particularly those who cannot be vaccinated for health reasons. It’s a matter of collective responsibility. Healthcare workers, the public, the states, public officials, NGOs – everyone has a role to play in protecting public health.
VT: Are there any positive European case studies where rubella has been wiped out?
NE: The Scandinavian countries have a very strong routine immunisation programme, a very strong health system, and high quality surveillance data. It looks like they have achieved elimination but we need to verify that. The WHO has started the verification process which involves examining national data in detail. According to surveillance data, all Scandinavian countries have low or no cases.
Denmark had two cases in 2008; the last rubella case in Finland was a single case in 2006; Sweden had three in 2010; and the last one in Norway was an isolated case in 2008 which we think may have been imported.
VT: Coming out of the Rome conference, what are the next steps in pushing for rubella elimination across Europe?
NE: We’ll continue to provide technical support for countries but the major event on the horizon is the European Immunization Week which will be a chance to raise awareness of measles and rubella vaccination. European Immunization Week takes place at the end of April.





VaccinesToday (@VaccinesToday) (@VaccinesToday) (@VaccinesToday) (@VaccinesToday)
February 24th, 2012
Why can’t Europe beat rubella? http://t.co/fFN9esQS #rubella #vaccines #CRS @WHO_Europe @ECDC_EU #pregnancy #birth #parenting #interview
VaccinesToday (@VaccinesToday) (@VaccinesToday) (@VaccinesToday) (@VaccinesToday)
February 24th, 2012
The US did it, Cuba did it – so why can’t Europe beat rubella? http://t.co/fFN9esQS #rubella #mmr #vaccines #Europe