There’s a lot riding on the ‘R’ – or reproductive number – of the novel coronavirus (SARS CoV2) which causes COVID-19. As the number rises and falls, ‘lockdowns’ and restrictions will tighten or ease.
It could determine how quickly people return to work, whether you go on holiday, and when to reopen schools. Crucially, it might be the reason we find ourselves in some form of lockdown again six months down the road.

The reproductive number is the average number of people who will contract a transmissible infection from one person with the disease. If that number is 1, it means someone with the virus will pass it to one person. If it’s two, each infected person will pass it to two people, who will each give it to two more people, and so on.
If the number is greater than 1, the number of people with the virus will rise; if it’s less than 1, the number is in decline.
Early in the coronavirus outbreak, experts were keen to know the R0 (pronounced ‘R nought’) – the number of people infected with the virus where there is no immunity. This is a measure of how infectious the disease is when no measures are taken to prevent its spread and nobody has recovered from the illness or received a vaccine.
However, while R0 represents the ‘natural’ infectiousness of a new bug, the effective reproductive number (sometimes written as Re or simply as R) tells us how many new cases are likely to be caused by each existing case. That is, how many people will catch the virus now, given that some people might be immune and/or social distancing measures are in place.

It’s inaccurate to talk about the R0 of coronavirus now that the world has responded with containment measures and some people have developed immunity. However, as politicians had already got their head around the term R0, they seem reluctant to ditch in favour of the more accurate ‘R’.
This is how Angela Merkel explained the effect of a higher #covid19 infection rate on the country’s health system.
This part of today’s press conf was great, so I just added English subtitels for all non-German speakers. #flattenthecurve pic.twitter.com/VzBLdh16kR
— Benjamin Alvarez (@BenjAlvarez1) April 15, 2020
This is a bugbear for Dr Peter English, a public health consultant and member of the Vaccines Today Editorial Board. In his blog on the topic, Dr English also explains why keeping R as low as possible could end the pandemic. While R < 1 means the outbreak is shrinking, keeping it to 0.5 is significantly better than holding it at 0.9. The former would see cases fizzle out by August; the latter mean we are living with new cases every day until March 2021.
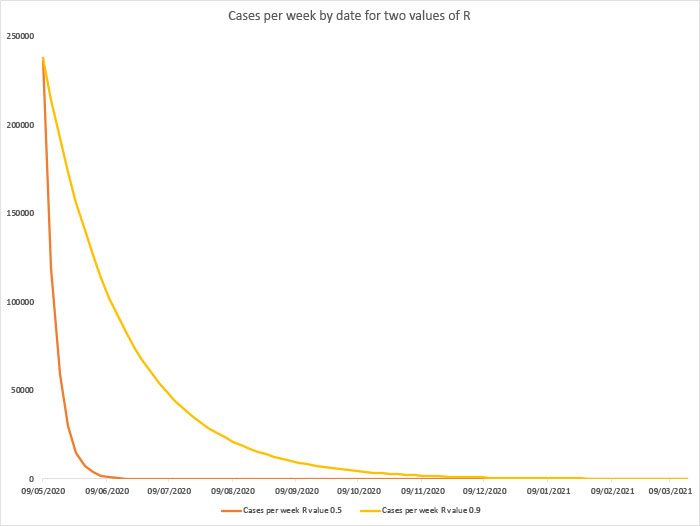
In reality, it is possible that R will bounce back up and in the months ahead, prompting tweaks in public health policy along the way. Germany and South Korea are among the many countries to have brought their R below one, only to see it rise above one after restrictions are eased.

We are all epidemiologists now
During the global financial crisis a decade ago, public interest in debit, deficits and bond markets increased. Financial literacy grew; suddenly we were all economists. Perhaps we can hope for greater understanding of infectious diseases and how they spread.
One of the knock-on effects of the growing interest in R0 is (a) that we can compare the infectiousness of SARS CoV2 to other viruses and (b) we are witnessing in real-time, how immunity and other measures can contain viruses.
The most common comparison you’ll find in the media today is between the novel coronavirus and influenza. R0 for coronavirus was estimated early in the pandemic to be between 2 and 2.5. Flu is roughly half that. The H1N1, for which we initially had no vaccine when it first emerged, is estimated to have an R0 of 1.2-1.6.
SARS (R0 = 4) and MERS (R0 = <1) which are also coronaviruses, illustrate how variable this class of viruses can be in their ability to spread.

The new coronavirus also has a higher R0 than Ebola where each person with the virus infects two others, in the absence of disease control measures. In the 1980s, HIV’s R0 was estimated to be 4 – although the Re is now far lower thanks to better understanding of how the disease spreads and the development of antiviral medicines.
But what about the infectious diseases for which we currently have vaccines? What is their R0?
- Smallpox has an R0 of 3
- Polio has an R0 of 4-6
- Mumps has an R0 of 10-12
- Chickenpox has an R0 of 10-12
- Pertussis has an R0 of 15-17
- Measles has an R0 of 16-18
This explains why measles elimination requires such a high level of immunity in the population. WHO and national health experts say two doses of measles-containing vaccines (MMR or MMRV) for 95% of the population are needed to stop the spread of the disease. In the absence of high uptake of the vaccine, even in small pockets of the community, outbreaks will occur.
The (relatively) good news is that SARS-Cov2 is much less transmissible than measles. We won’t need 95% immunity to stop its spread. And other containment measures, such as social distancing, clearly have a significant impact on its effective R. But, unlike MERS, it is likely that continued outbreaks will occur if the virus is given the opportunity.






Pingback
December 9th, 2021
[…] symptoms right away, and a single person unaware that they have measles can spread it to between 16-18 other people (what is called the R0). It requires vaccination to not only create herd immunity to prevent the spread of the virus, but […]
Pingback
December 10th, 2021
[…] immunity is lower than if a virus is highly contagious. The level of infectious is recorded in the reproductive number, or R0, which records the average number of people an infected person […]
Simon Trevant
March 16th, 2022
I’m fascinated with how this article has dated. I believe I read that the new BA.2 COVID variant is an R factor of 1:12, as infectious as Chickenpox?
Gary Finnegan
March 21st, 2022
Good point Simon. We will review this.
Ray Kamada
April 29th, 2022
SARS-COV-2 started with an R0 ~2.6, according to estimates from Wuhan and an age-normalized synthesis of Diamond Princess cruise ship data. So, in 2.5 years it’s quickly mutated to the soon to be dominant variant, BA.2.12.1, which, according to New Delhi public health, is 30 to 90% more contagious than its most recent major predecessor, BA.2, which had an R0 of ~12, which then puts BA.2.12 at an R0 of something like 16 to 22.
That suggests we have a new “King of the Hill”. That is, under unconstrained conditions, covid is now the most humanly transmissible disease on Earth.
The speed with which it accomplished this astounding feat, the fact that asymptomatic and pre-symptomativ hosts can readily transmit this disease, which also features the form known as Long Covid, and that, unlike measles, it can keep re-infecting people, over and over again, in as little as less 3 weeks, and that it’s often a seriously debilitating, even lethal disease, without being so lethal as to curtail its transmission significantly, suggests to me that it’s by far the most perfect human scourge that nature has ever developed. Indeed, if reports in the mainstream media didn’t keep dissing the notion, its very perfection might lead one to suspect that some virological gain-of-function research has produced wildly spectacular, in vivo, results.
Pingback
May 19th, 2022
[…] no pertussis, but this ain’t no fooling around. Influenza, in comparison runs an R0 slightly less than 2. Infectious diseases has always been evolution in action, and evolution in COVID is scary quick. […]
Pingback
May 20th, 2022
[…] Famously, the r0 for the Omicron variant of SARS-CoV2 could be as high as 8-12. Whereas, chickenpox probably has an r0 of 10-12, and measles 16-18. […]
Pingback
June 11th, 2022
[…] per infection) than measles (12-18 transmissions) and chickenpox (10 transmissions), but similar to polio (4-6 transmissions). The case mortality rate for COVID-19 (0.008%) is less than that for […]
Pingback
June 26th, 2022
[…] this ain’t no pertussis, but this ain’t no fooling around. Influenza, in comparison runs an R0 slightly less than 2. Infectious diseases have always been evolution in action, and evolution in COVID is scary quick. […]
Pingback
September 12th, 2022
[…] I know that locking down hard is not the answer. But the new Covid BA.2 variant is said to have a reproduction number (R) of 18 – one of the most contagious viruses documented to date. When the R number is that […]
Pingback
September 21st, 2022
[…] Vaccines Today explains, a virus’s reproductive rate or R0 (pronounced “R naught”) indicates how […]
Pingback
September 23rd, 2022
[…] Vaccines Today explains, a virus’s reproductive rate or R0 (pronounced "R naught") indicates how […]
Jin
April 25th, 2023
Hi, can you share the reference of “Polio has an R0 of 4-6”? Thank you.
Gary Finnegan
May 9th, 2023
Some estimates put it at ‘5-7’
Doherty M., Buchy P., Standaert B., Giaquinto C., Prado-Cohrs D. Vaccine impact: benefits for human health. Vaccine. 2016;34:6707–6714. doi: 10.1016/j.vaccine.2016.10.025.
Pingback
March 23rd, 2025
[…] in your sensory nerve ganglia and sometimes comes back as shingles! Yippee! Chicken Pox has an R0 of 10-12 which is slightly less contagious than measles, but still highly transmissible. There’s a reason […]