This article was first published by Chatham House and is cross-posted here with permission.
On 10 January 2020, Chinese scientists released the sequence of the COVID-19 genome on the internet. This provided the starting gun for scientists around the world to start developing vaccines or therapies. With at least 80 different vaccines in development, many governments are pinning their hopes on a quick solution. However, there are many hurdles to overcome.
Vaccine development
Firstly, vaccine development is normally a very long process to ensure vaccines are safe and effective before they are used.
Safety is not a given: a recent dengue vaccine caused heightened disease in vaccinated children when they later were exposed to dengue, while Respiratory Syncytial Virus vaccine caused the same problem.
Nor is effectiveness a given. Candidate vaccines that use novel techniques where minute fragments of the viruses’ genetic code are either injected directly into humans or incorporated into a vaccine (as is being pursued, or could be pursued for COVID-19) have higher risks of failure simply because they haven’t worked before.
For some vaccines, we know what levels of immunity post-vaccination are likely to be protective. This is not the case for COVID-19. Clinical trials will have to be done for efficacy. This is not optional – regulators will need to know extensive testing has taken place before licencing any vaccine. Even if animal tests are done in parallel with early human tests, the remainder of the process is still lengthy.
There is also great interest in the use of passive immunization, whereby antibodies to SARS-CoV-2 (collected from people who have recovered from infection or laboratory-created) are given to people who are currently ill. Antivirals may prove to be a quicker route than vaccine development, as the testing requirements would be shorter, manufacturing may be easier and only ill people would need to be treated, as opposed to all at-risk individuals being vaccinated.
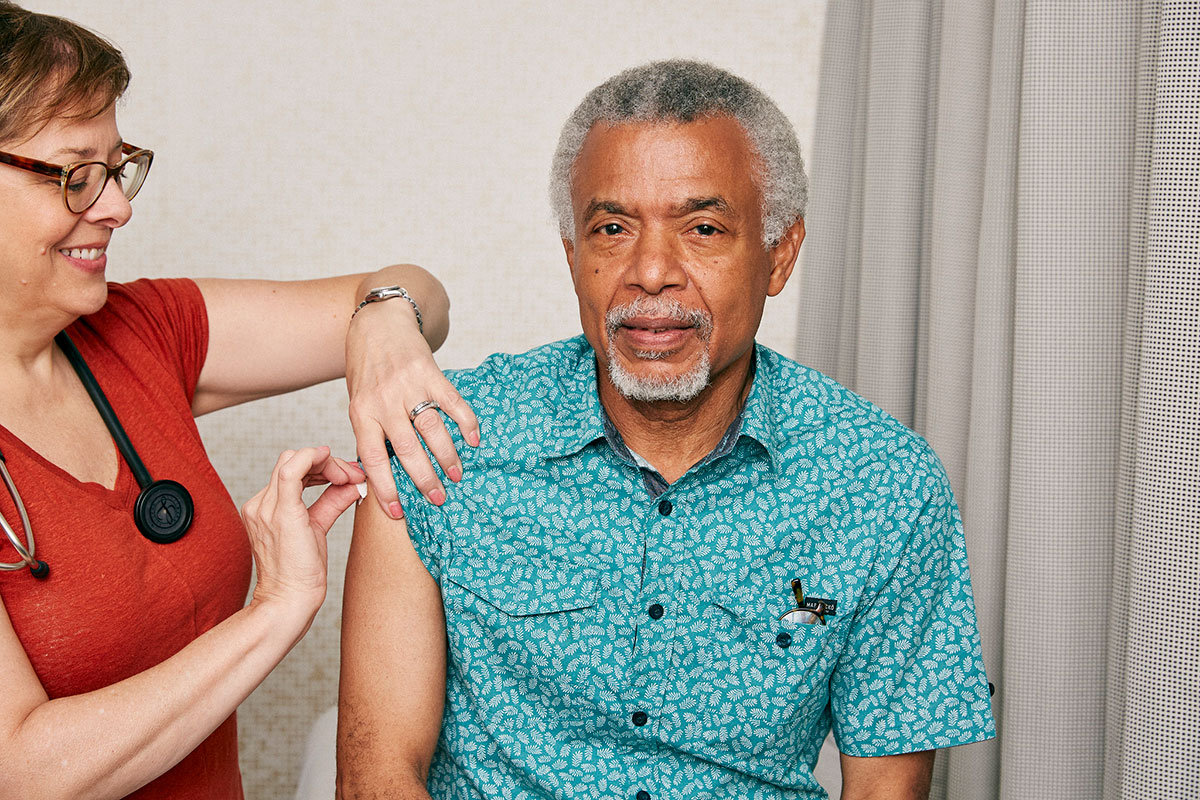
Vaccine manufacturing
Developers, especially small biotechs, will have to make partnerships with large vaccine manufacturers in order to bring products to market. One notorious bottleneck in vaccine development is getting from proof-of-principle to commercial development: about 95 per cent of vaccines fail at this step. Another bottleneck is at the end of production. The final stages of vaccine production involve detailed testing to ensure that the vaccine meets the necessary criteria and there are always constraints on access to the technologies necessary to finalize the product. Only large vaccine manufacturers have these capacities. There is a graveyard of failed vaccine candidates that have not managed to pass through this development and manufacturing process.
Another consideration is adverse or unintended consequences. Highly specialized scientists may have to defer their work on other new vaccines to work on COVID-19 products and production of existing products may have to be set aside, raising the possibility of shortages of other essential vaccines.
Cost is another challenge. Vaccines for industrialized markets can be very lucrative for pharmaceutical companies, but many countries have price caps on vaccines. Important lessons have been learned from the 2009 H1N1 flu pandemic when industrialized countries took all the vaccines first. Supplies were made available to lower-income countries at a lower price but this was much later in the evolution of the pandemic. For the recent Ebola outbreaks, vaccines were made available at low or no cost.
Geopolitics may also play a role. Should countries that manufacture a vaccine share it widely with other countries or prioritize their own populations first? It has been reported that President Trump attempted to purchase CureVac, a German company with a candidate vaccine. There are certainly precedents for countries prioritizing their own populations. With H1N1 flu in 2009, the Australian Government required a vaccine company to meet the needs of the Australian population first.
Vaccine distribution
Global leadership and a coordinated and coherent response will be needed to ensure that any vaccine is distributed equitably. There have been recent calls for a G20 on health, but existing global bodies such as the Coalition for Epidemic Preparedness Innovations (CEPI) and GAVI are working on vaccines and worldwide access to them. Any new bodies should seek to boost funding for these entities so they can ensure products reach the most disadvantaged.
While countries that cannot afford vaccines may be priced out of markets, access for poor, vulnerable or marginalized peoples, whether in developed or developing countries, is of concern. Developing countries are at particular risk from the impacts of COVID-19. People living in conflict-affected and fragile states – whether they are refugees or asylum seekers, internally displaced or stateless, or in detention facilities – are at especially high risk of devastating impacts.
Mature economies will also face challenges. Equitable access to COVID-19 vaccine will be challenging where inequalities and unequal access to essential services have been compromised within some political systems.
The need for global leadership
There is an urgent need for international coordination on COVID-19 vaccines. While the WHO provides technical support and UNICEF acts as a procurement agency, responding to COVID-19 needs clarity of global leadership that arches over national interests and is capable of mobilizing resources at a time when economies are facing painful recessions. We see vaccines as a salvation but remain ill-equipped to accelerate their development.
While everyone hopes for rapid availability of safe, effective and affordable vaccines that will be produced in sufficient quantities to meet everyone’s needs, realistically, we face huge hurdles.
Professor David Salisbury is an Associate Fellow, Global Health Programme at Chatham House, and a member of the Vaccines Today Editorial Board
Dr Champa Patel is Director, Asia-Pacific Programme at Chatham House



