Sometimes we take progress for granted. For decades, the number of children receiving their basic immunisations rose steadily. There were still ‘zero dose’ children ‒ kids who, due to poverty and lack of access to health services, received no vaccines ‒ but the number was falling.
Now the trend has reversed.
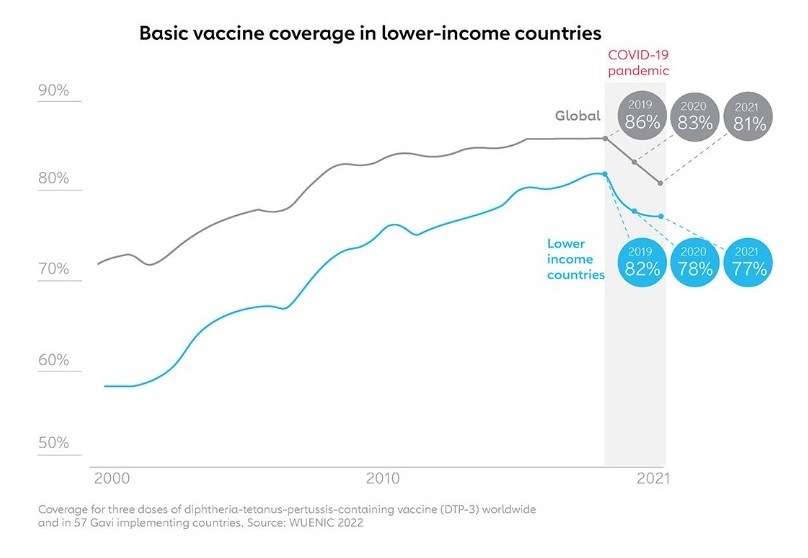
The WHO and UNICEF have reported the largest sustained decline in childhood vaccinations in 30 years. The percentage of children who received three doses of the vaccine against diphtheria, tetanus and pertussis (DTP3) fell 5 percentage points between 2019 and 2021 to 81%.

There are now 25 million children who missed out on one or more doses of DTP through routine immunisation services in 2021 alone ‒ an increase of 2 million compared to 2020 and an increase of 6 million compared to 2019. This leaves them at real risk from devastating but vaccine-preventable diseases.
There has also been a resurgence in meningitis, reports of polio cases and outbreaks of measles, arising from missed immunisations. Zimbabwe alone has reported 6,551 measles cases and 704 measles-related deaths. These illnesses are preventable but will continue without urgent action.
The decline in vaccination is attributed to service disruptions arising from COVID-19, the increase in vaccine misinformation, and the growing numbers of families affected by conflict and migration.
‘This is a red alert for child health,’ said Catherine Russell, UNICEF Executive Director. ‘We are witnessing the largest sustained drop in childhood immunisation in a generation. The consequences will be measured in lives.’
Russell said that while a ‘pandemic hangover’ was expected as a result of COVID-19 disruptions, this is not an excuse for the ongoing decline. She called for immunisation catch-up campaigns to reach millions of vulnerable children before new outbreaks of disease begin to add to pressure on health services.
‘Planning and tackling COVID-19 should also go hand-in-hand with vaccinating for killer diseases like measles, pneumonia and diarrhoea,’ said Dr Tedros Adhanom Ghebreyesus, WHO Director-General. ‘It’s not a question of either/or, it’s possible to do both’.

There are also challenges with human papillomavirus (HPV) vaccines which protect against cervical cancer and other diseases. Over a quarter of HPV vaccine coverage achieved in 2019 has been lost. This exacerbates major global inequalities and is likely to lead developed countries to eliminate the disease in the coming decades while poorer countries lag behind.
There were some bright spots in the data, such as sustained high levels of coverage reported by Uganda’s routine immunisation programme. Similarly, Pakistan has returned to pre-pandemic levels of coverage, thanks in part to catch-up programmes.
In the 57 countries supported by Gavi, the vaccine alliance, basic vaccine coverage fell by just one percentage point. Gavi said two-thirds of African countries have shown clear signs of recovery.
‘It’s heart-breaking to see more children losing out on protection from vaccine-preventable diseases for a second year in a row,’ said Dr Seth Berkley, CEO of Gavi, the Vaccine Alliance. ‘The priority must be to help countries to maintain, restore and strengthen routine immunisation alongside executing ambitious COVID-19 vaccination plans, not just through vaccines but also tailored structural support for the health systems that will administer them.’

WHO and UNICEF are working with Gavi and other partners to deliver the global Immunisation Agenda 2030 (IA2030), a strategy for all countries and relevant global partners to achieve set goals on preventing diseases through immunisation and delivering vaccines to everyone, everywhere, at every age.
Top of their ‘to do’ list will be an urgent effort to stop the growth in the number of zero-dose children who have not been vaccinated at all. Then, as 2030 approaches, the global goal will be to regain momentum and drive down rates of vaccine-preventable disease.
In short, it’s time to restore progress.





Pingback
April 25th, 2023
[…] la pandemia de COVID-19 se sigue sintiendo en los países con las tasas de vacunación más bajas. Millones de niños se han quedado sin vacunasCon algo – dosis cero niños, que no recibieron ninguna de las inyecciones […]