Rubella (‘German measles’) is an infectious disease that can be prevented by the MMR vaccine, which also protects against measles and mumps. Infection is usually mild but the virus can cause severe birth defects if contracted during pregnancy.
Read: Congenital Rubella Syndrome – Ian’s Story
As rubella is less infectious than measles, there are far fewer cases in Europe – except in one country: Poland.
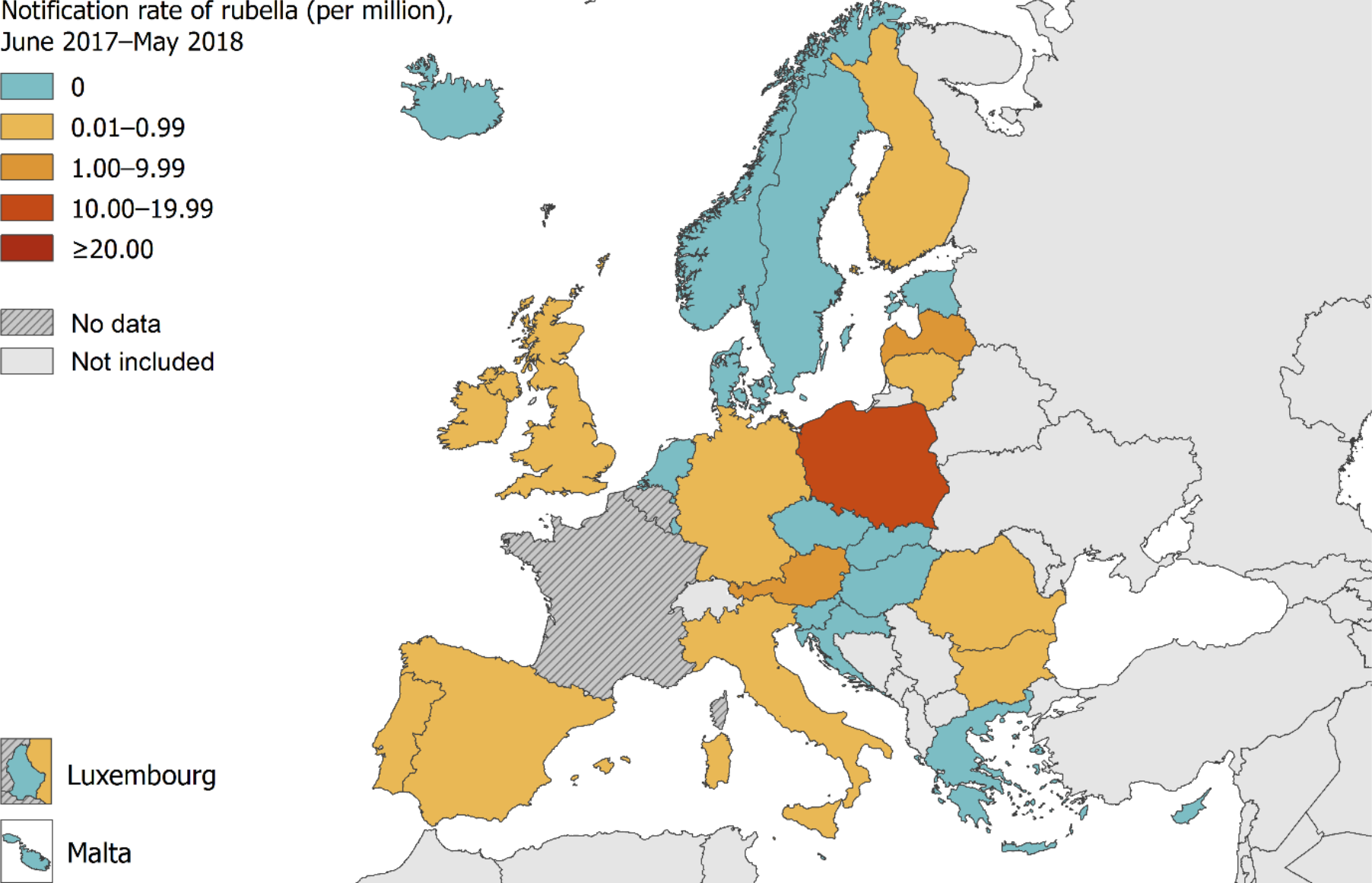
Data from the European Centre for Disease Prevention & Control (ECDC) show than 620 cases of rubella were recorded in 13 EU/EEA countries reporting cases from 1 June 2017 and 31 May 2018. Some countries did not submit reports and others (Belgium and France) do not report rubella cases to the system at all. Of those that do, many recorded no cases at all.
Where cases were reported, numbers were low – at least compared to measles for the same period. Austria (21), Germany (63) and Italy (30) all reported small outbreaks.
Meanwhile, Poland had 481 cases in the same 12-month period. What’s more, the number of cases in May 2018 – the latest month for which there is data – is the highest all year. There were 60 cases in May 2018.
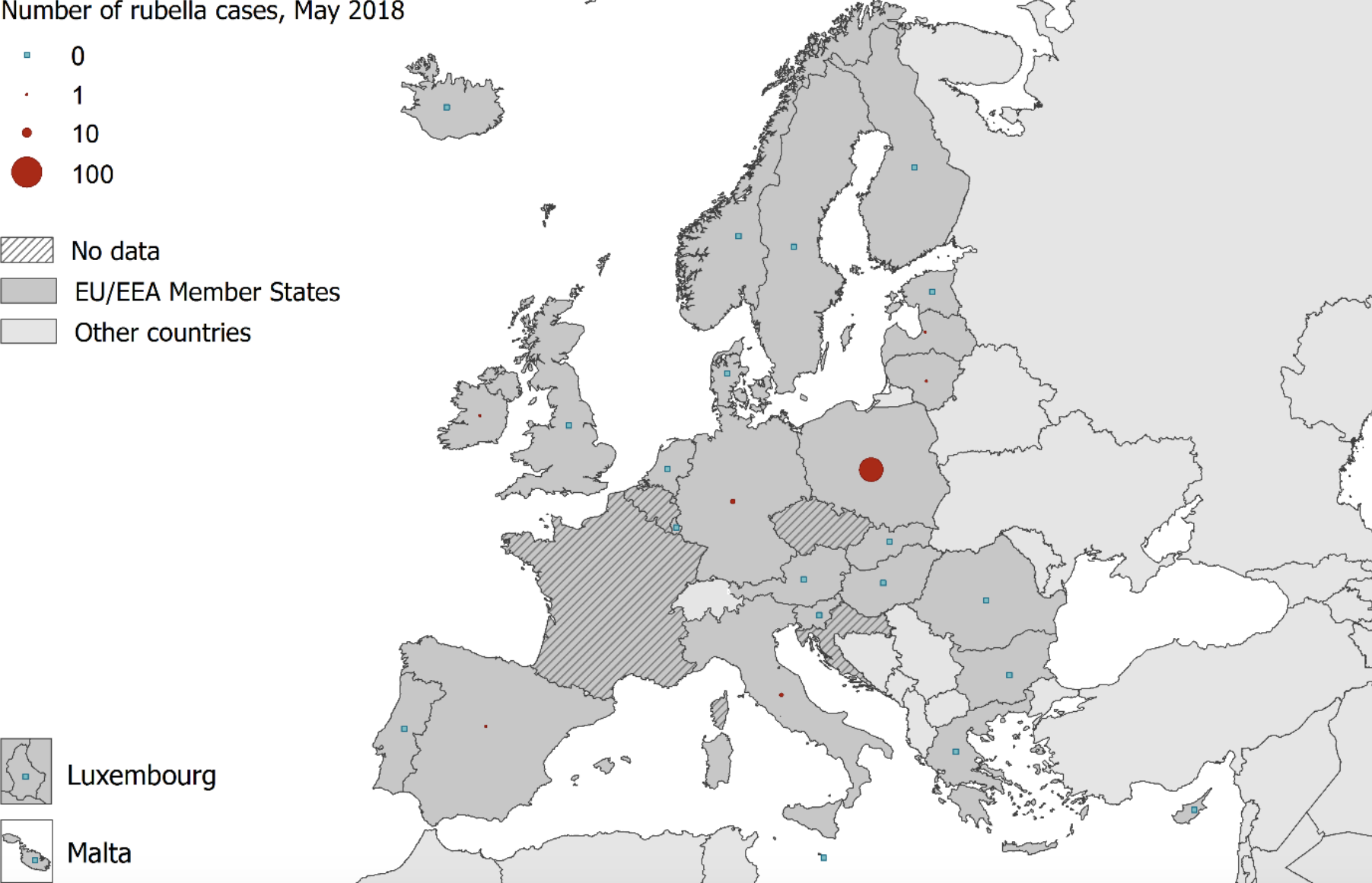
So, what is going on?
First, some history. Between 1989 and 2004, only adolescent girls in Poland were vaccinated against rubella. The thinking behind this practice (which was common in several European countries) was that rates of congenital rubella syndrome (CRS) could be reduced by vaccinating young women.
This has a certain logic but left young men unprotected, meaning the virus continued to spread in the community. Since 2004, a universal two-dose MMR vaccination programme for boys and girls has been in place in Poland. Vaccination rates in Poland are above the European average.
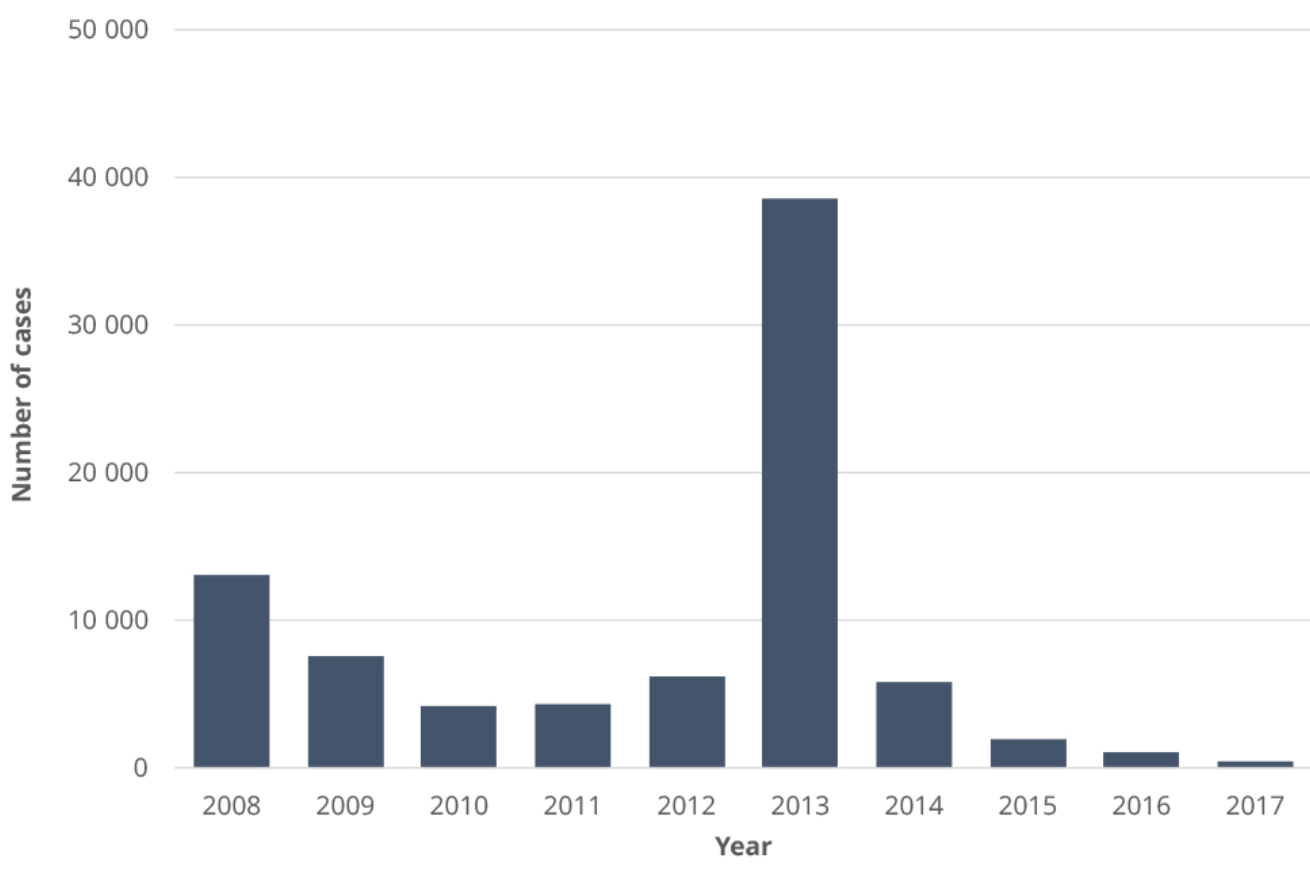
Still, outbreaks among adolescents and young adult males occur frequently in Poland including a severe epidemic in 2013. This increases the risk of pregnant women contracting the disease, leading to congenital rubella syndrome (CRS).
However, that may not fully explain the apparently high rates of rubella in Poland. While rubella is rarely seen in most EU countries – and doctors have therefore very little experience with the symptoms – GPs in Poland remain sensitive to rashes and other signs of the disease.
Suspected cases are swiftly reported by diligent doctors. But not all of these ‘cases’ are rubella infections. According to Polish laboratory services, over 90% of suspected cases test negative for rubella. ‘This probably means that physicians reporting based on clinical symptoms are wrong – most reported rubella cases are not rubella,’ said Prof Wlodzimierz Gut, the Head of the Measles and Rubella Reference Laboratory from National Institute of Public Health – National Institute of Hygiene.
There is an ongoing discussion among experts in Poland on the necessary introduction of case-based surveillance including laboratory confirmation of every rubella suspicion. This type of reporting is now recommended by WHO for all European countries and requires enhancement of laboratory capacity.
Ready more about rubella in Poland on the Szczepienia website.





