Since the outbreak of war in Syria in 2011, Lebanon has cared for more refugees than any country in the world. At the beginning of their neighbour’s civil war, the Lebanese population was just over 5 million, including almost half a million Palestinian refugees. Today, an estimated 6.8 million live in Lebanon, including around 1.5 million people from Syria.
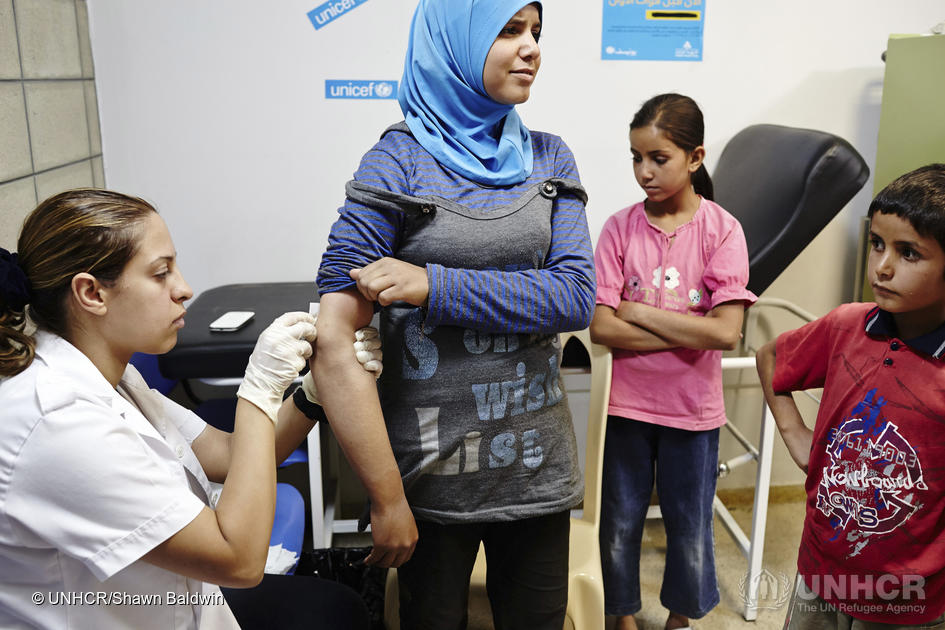
The public health response was swift: any child crossing the Lebanon-Syria border in the years after 2011 was vaccinated against measles and polio. Children are referred to the primary care network for immunisation and development checks.
The UN Refugee Agency (UNHCR) subsidises a package of primary care services, but the situation poses challenges for the infrastructure of a small country. Despite this, Lebanon continues to prioritise preventative care, including vaccination. However, new stresses are on the horizon as COVID-19 takes hold and donor support dries up.
‘We estimate that one in every four people in Lebanon is a refugee,’ says Dr Randa Hamadeh, Manager of the Vaccination Programme in Lebanon. ‘Two years ago, there was an estimated 2,250,000 people from Syria, including unofficial entries who had not registered. Now it has settled down to around 1.5 million.’
Large numbers of those who fled the conflict live in tented settlements, but many others were seasonal workers who opted to stay on in Lebanon rather than return to Syria. They live in towns and cities around Lebanon and many have welcomed their wider family as the situation in Aleppo, Raqqa, Homs and other Syrian cities deteriorated dramatically.
‘This can pose additional challenges for communities and for the health system, particularly as people are integrated into local towns and schools, but may not be registered,’ Dr Hamadeh explains. ‘We have to go into every community if we want to reach people and make sure we don’t have polio cases. We have been polio free for 16 years and want to keep it that way.’
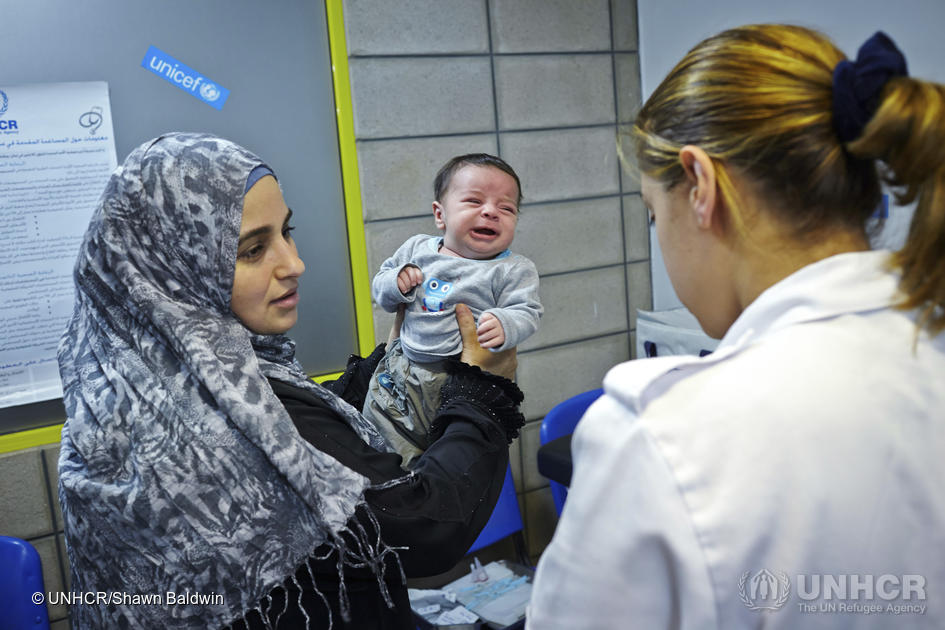
Like Lebanon, Syria is one of the most developed countries in the region and, at least until war broke out, had a robust health and immunisation system. However, immunisation records are often lost or incomplete and conditions in camps mean infectious diseases can spread quickly in the absence of herd immunity.
A long decade
With the Syrian conflict entering its 10th year, new challenges are emerging. Lebanon’s response to the emergency saw an unprecedented level of neighbourly solidarity, coupled with support from international agencies. But with no end in sight, and new challenges arising from outbreaks of COVID-19, the strain is showing. Lebanese people are growing weary of responding to an interminable crisis not of their making, and international agencies are distracted by a global pandemic.
‘It put a lot of pressure on our systems, especially at the beginning, but with the support of the international community it was affordable,’ Dr Hamadeh says.

‘Now we have donor fatigue. Some funding comes with conditions attached; other previously reliable sources are drying up. We cannot get enough funding for vaccination. The EU provided €6 million every two years, through a multi-donor trust, for vaccination programmes and essential drugs. But now the Lebanese government is subsidising the procurement of vaccinations and we need to increase the fund to meet demand.’
When vaccines are covered by donations, Lebanon often has to shoulder the burden of storing, distributing and administering them. There is a lot at stake, not least the global effort to eradicate polio. However, the pressure on systems and resources can cause social and political strain.
‘More Lebanese people are living in poverty and we’ve also seen a rise in the number of measles cases which prompted us to launch a new national MMR campaign for people aged from six months to 10 years,’ she says. ‘The measles outbreak will peak soon but, at the same time, coronavirus is shifting attention and we are struggling to deal with the additional demand on primary healthcare services.’

Stress on the health system seems unlikely to ease any time soon. Syria too is grappling with outbreaks of coronavirus but many of its public services have collapsed. More people may flee Syrian cities for Lebanon, Turkey, Jordan and Egypt.
‘What happens in the years to come is a political question. We cannot say when it will be safe for people to return to Syria and how many will want to,’ Dr Hamadeh says.
‘We are likely to live under very stressed conditions in the long-term. Even the demographics suggest demand will rise. Syrian people in Lebanon are generally young: the annual birth cohort of the Lebanese population is 73,000; among Syrians [in Lebanon], it was 62,000.’
As Syrians are a minority, their proportional contribution to population growth is significant. This means more children will need access to vaccination and other childhood health services to give them the best chance of long-term health.
Expanding universal services
In addition to offering a package of free services to refugees, Lebanon has stepped up its universal healthcare and subsidised social services for poorer Lebanese people.
Along with improving the lives of citizens, the move is partly designed to reduce resentment and discrimination against people who have arrived from Syria over the past decade.

‘More funds are needed for basic primary healthcare,’ says Dr Hamadeh. ‘We are not asking anyone to help Lebanese people – we can manage this from our resources. What we need is for the international community to take care of those who are in Lebanon and need support. We all share an interest in making this work.’




