If you are one of the billions of people who have to receive a COVID-19 vaccine, you have had an intramuscular injection. The needle was almost certainly inserted at a 90° angle into the deltoid muscle at the top of your arm/shoulder.
This way of delivering vaccines is used in most vaccines, but it is not the only way to administer vaccines.
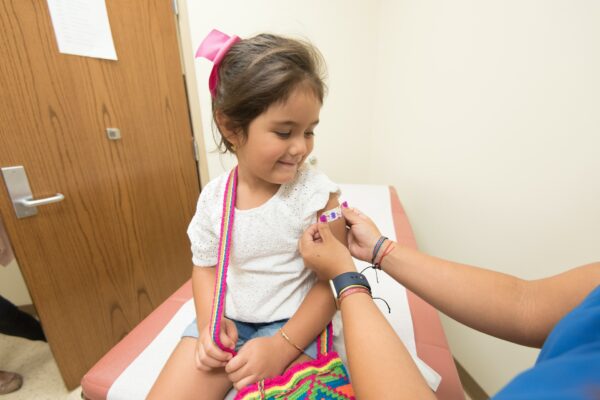
For example, MMR vaccines (against measles, mumps and rubella) are usually administered by subcutaneous injection, into the layer of tissue above the muscle (i.e. it’s not as deep as intramuscular vaccination). The BCG vaccine (against tuberculosis) can be given intradermally into the outer layer of the skin.
There are other options too: some polio vaccines are given orally (by mouth), an intranasal spray is used to give some flu vaccines, and researchers continue to study the use of nanopatches to deliver vaccines painlessly (although no such vaccine is currently available).
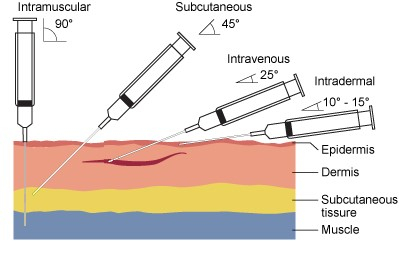
Source: British Columbia Institute of Technology (Wikipedia)
Given the range of options, and the temporary sore arm you may have experienced after your vaccines, you might wonder why injecting deep into muscle tissue is still the most common way to administer vaccines. Why aren’t COVID vaccines sprayed up the nose where SARS-CoV-2 often enters, or injected into the bloodstream where it can be transported around the body?
The short answer is that intramuscular vaccination is, for most kinds of vaccine, still the most effective, safe and well tolerated.
For a start, muscle is rich in immune cells that can recognise antigens (such as the SARS-CoV-2 virus spike protein which is targeted by most COVID-19 vaccines) and carry them to lymph nodes. Lymph nodes are important parts of the immune system which contain cells that create antibodies that prevent viruses from entering human cells or activate immune cells that destroy cells already infected by viruses.
The deltoid muscle in your shoulder is located close to the armpit which is a good source of lymph nodes. In contrast, fat tissue does not have such a good blood supply or connections to lymph nodes and is less effective at absorbing vaccines.
Injecting vaccines into the body always causes some inflammation. Another benefit of using muscle is that it keeps this inflammation ‘local’. This means that while you may have a sore arm, the inflammation is generally confined to the area into which the vaccine was injected. In contrast, injecting directly into the bloodstream could trigger a more general undesired response.
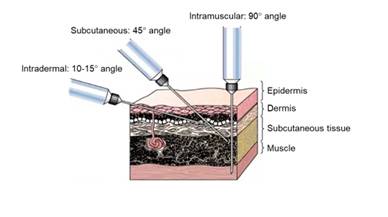
Perhaps counterintuitively, injecting vaccines deep into muscle tissue is less painful than injecting into the outer layers of skin. That’s because most pain fibres are near the surface of the skin.
Still, if you have a fear of needles, or would simply prefer a more convenient and comfortable way to be protected from infection, you’ll be pleased to hear that researchers are exploring a range of options including ‘gene guns’ for DNA vaccines, microneedles, and inhaled vaccines.
While some of those technologies are in early trials, none is yet available to you. Until then, you’ll have to roll up your sleeves.
This information is provided for information purposes and should not be viewed as medical advice. Speak to your healthcare provider if you have individual questions about vaccination.




Peter Gray
February 9th, 2022
I am curious why Intradermal injections are not being utilized for COVID vaccination, and if they are used; it should bestow better immunity, should it not?
Gary Finnegan
February 11th, 2022
The short answer is that intramuscular vaccination is, for most kinds of vaccine – including COVID-19 vaccines – the most effective, safe and well tolerated.
The longer answer:
Muscle is rich in immune cells that can recognise antigens (such as the SARS-CoV-2 virus spike protein which is targeted by most COVID-19 vaccines) and carry them to lymph nodes. Lymph nodes are important parts of the immune system which contain cells that create antibodies that prevent viruses from entering human cells or activate immune cells that destroy cells already infected by viruses.
The deltoid muscle in your shoulder is located close to the armpit which is a good source of lymph nodes. In contrast, fat tissue does not have such a good blood supply or connections to lymph nodes and is less effective at absorbing vaccines.
Injecting into the muscle is, perhaps surprisingly, not as painful as injecting into the outer layers of skin because most pain fibres are near the surface of the skin.
Jay
February 10th, 2022
Somebody told me a dentist can inject the covid-19 vaccine in your mouth, like they do novocaine. Is this true?
Gary Finnegan
February 11th, 2022
That’s not the approved and recommended route of administration. It is designed to go into a muscle rather than your mouth or gums.